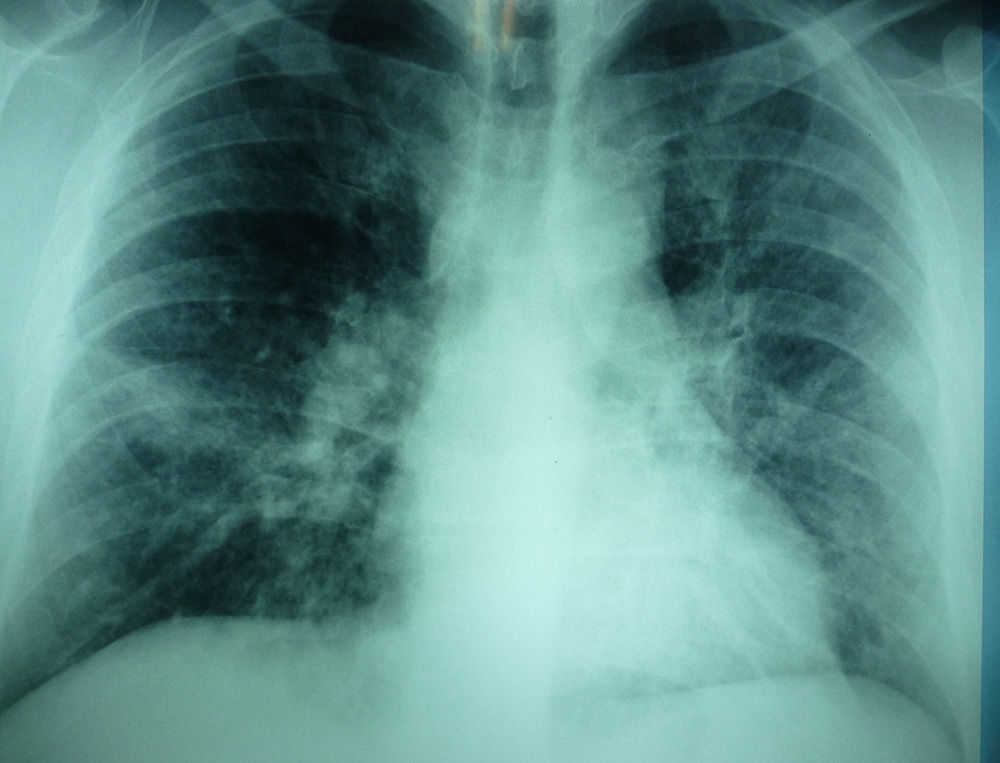
A 39-year-old man (heavy smoker, hypertensive and moderately obese) presented at the Internal Care Unit in October 2012 suffering from a 3-day history of dyspnea, paroxysmal productive cough and retrosternal pain, with no fever. Scarce end-expiratory crackles in middle and lower lung fields bilaterally with associated mildly prolonged expiratory phase of respiration and mild leucocytosis were recorded. The patient refused hospitalization, and two days later he returned due to worsened, intense dyspnea at rest, heart rate of 130/min and fever (38.5°C). A new chest X-ray revealed more intense alveolar infiltrates, diffuse and expanded throughout the whole left lung and the right middle lung field (Fig. 1). Routine blood tests showed leukocytosis, elevated neutrophiles and monocytes, relatively increased CRP (7.5mg/dl), ESR (73mm/h), ALT (83U/L) and LDH (484U/L).
The patient was administered levofloxacin, piperacillin/tazobactam, supplementary oxygen, inhaled bronchodilators and oseltamivir (for 5 days) because influenza pneumonia could not be excluded; however, his condition deteriorated and non-invasive bi-level positive pressure ventilation was applied with full-face mask for 24h. Ten days later he was discharged completely recovered.
During hospitalization, 3 whole blood and serum samples (on second admission, at 21 days and one month later) were collected together with sputum, pleural fluid and urine samples. Sera were tested by IFA for IgM and IgG antibodies against L. pneumophila sg1, L. pneumophila sgs 2–14 and Legionella species (L. rubrilucens, L. anisa, L. brunensis, L. quinlivanii, L. maceachernii, L. oakridgensis, L. taurinensis and L. londiniensis) using a homemade slide. Sera tested positive for L. maceachernii IgG antibodies in all samples (first: 1/960, second: 1/3840, third: 1/3840); titers for remaining species and/or serogroups ranged from 0–1/480. IgM antibodies tested positive (1/50) only for the first sample and only for L. maceachernii. All sera tested negative for Hepatitis Viruses, HIV, Coxiella burnetii, Mycoplasma pneumoniae and Chlamydia pneumoniae.
DNA was extracted (Qiamp DNA blood mini kit, Qiagen, Hilden, Germany) from whole blood and sputum samples and was tested by multiplex Real-time PCR for L. pneumophila and Legionella species,1 which was positive, at low copy numbers, for Legionella species on the pleural fluid only.
An isolate, following culture (buffered charcoal yeast extract medium supplemented with α-ketoglutarate (BCYE-α) and BCYE with polymyxin B, anisomycin, and vancomycin petri dishes at 36°C/2.5% CO2) of whole blood pleural fluid and sputum samples was tested by MALDI-TOF MS (Bruker Daltonics) and matched Legionella species at a score of 1.99.
Legionella maceachernii infection is mostly expressed as pneumonia,2 although recently a case of soft-tissue infection by the pathogen was reported.3 All 6 patients described so far had underlying disorders, such as HIV infection, multiple myeloma, pulmonary fibrosis, systemic lupus erythematosus, and autoimmune hemolytic anemia, or had undergone liver transplantation. All but one patient died. Since the clearance of L. maceachernii from the lungs of infected mice has shown to be relatively quick compared to other species,4 the increased mortality might be due to the concomitant presence of an underlying disease.
Please cite this article as: Pasparaki E, Chochlakis D, Damianaki A, Psaroulaki A. Neumonía grave adquirida en la comunidad debida a infección por Legionella maceachernii. Arch Bronconeumol. 2015;51:97–98.