We report the case of a 50-year-old man, with no significant clinical history, who presented in an emergency department in the city of Cuzco with a 3-day history of nausea, vomiting, and progressive dyspnea. Chest X-ray revealed bilateral pleural effusion. Cytochemical analysis of the pleural fluid was consistent with empyema. The patient developed progressive respiratory failure requiring mechanical ventilation and transfer to the intensive care unit (ICU), where he was treated with wide-spectrum antibiotics and bilateral chest drainage. He was extubated 10 days later, and transferred to our ICU in Lima.
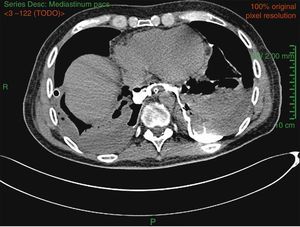
On arrival, his bilateral empyema persisted, so a computed tomography was performed with oral contrast medium, showing esophageal perforation (Fig. 1). The diagnosis of esophageal perforation was confirmed on upper endoscopy, showing an ogival-shaped rupture in the posterior esophageal wall communicating with the mediastinum 3cm from the gastroesophageal junction. The fistula was closed with metal clips and a nasojejunal tube was placed. The patient's progress was favorable, enteral nutrition was well tolerated, and no signs of sepsis or respiratory failure were observed. After placement of the clips, chest drainage reduced progressively to less than 100cc/24h. This situation was maintained until the patient was discharged and transferred to Germany to continue his recovery, where the clips were finally removed.
Boerhaave's syndrome is the spontaneous perforation of the esophagus due to a sudden increase in intraesophageal pressure.1 The non-specific nature of the symptoms may contribute to a delay in diagnosis and worsen prognosis. Pneumomediastium or pneumoperitoneum associated with pleural effusion, pneumothorax and/or subcutaneous emphysema are generally seen on chest X-ray.2 Diagnosis is confirmed by computed tomography, esophagogram with contrast medium, or endoscopy.
Please cite this article as: Makikado LDU, Rocca CAN, Malca GEG. Empiema bilateral secundario a una perforación esofágica espontánea. Arch Bronconeumol. 2016;52:166.