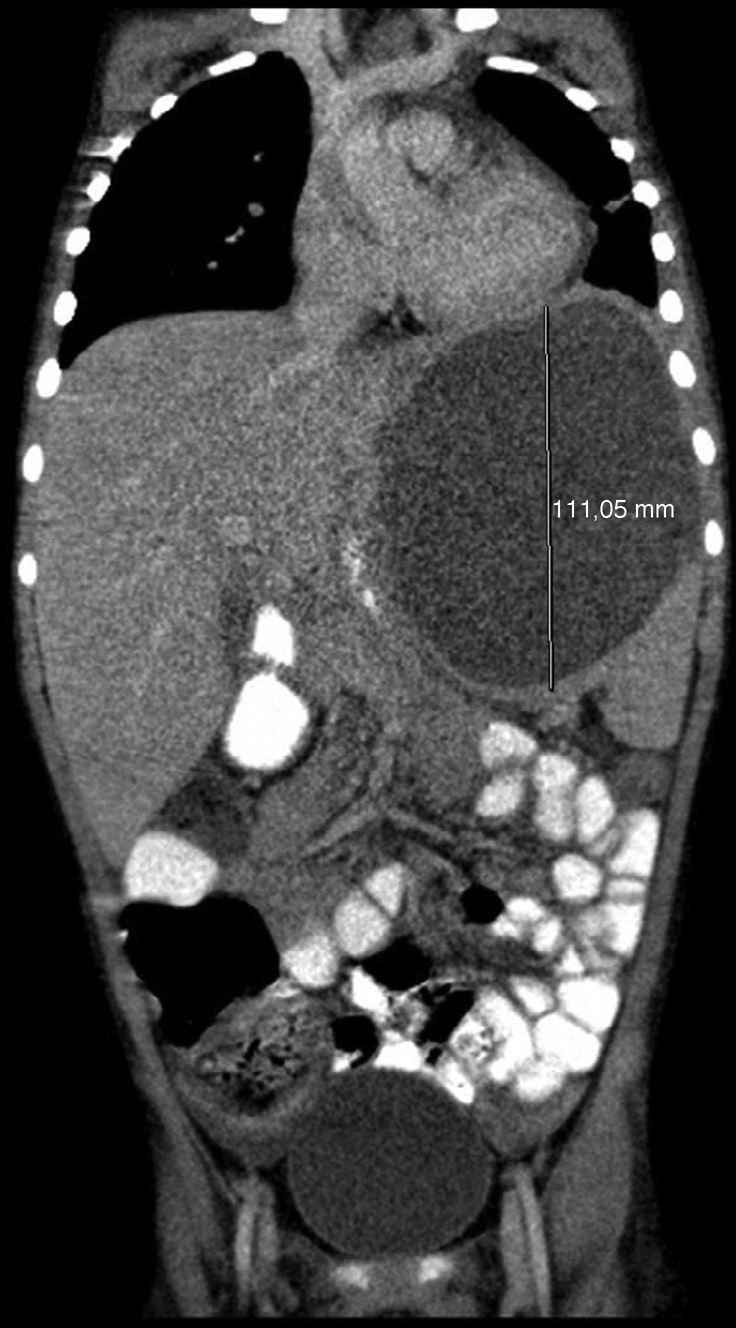
Splenic abscesses (SA) are unusual extraintestinal manifestations of salmonellosis, mainly due to S. typhi, S. typhimurium and S. paratyphi.1 These abscesses are difficult to diagnose due to their low incidence and nonspecific symptoms, and mortality is high if they are not treated early. They often develop on preexisting lesions, are directly related or secondary to hematologic disease, hemoglobinopathies or injuries, and present with concurrent bacteremia or endocarditis.2 Up to 80% of chest X-rays show changes, and up to 30% of cases involve left pleural effusion.3 We report the case of a 5-year-old patient presenting with short-term fever and abdominal pain 2 weeks after a diagnosis of gastroenteritis due to Salmonella spp. In view of suspected typhoid fever, intravenous ampicillin was administered (150mg/kg/day). Clinical laboratory test results showed leukocytes 24 580μl (neutrophils 21 150μl), C-reactive protein (CRP) 28.5mg/dl and procalcitonin 5.63μg/ml. Fever and hypoventilation in the left lung base persisted, so a chest X-ray was performed. Basal pneumonia with parapneumonic effusion was diagnosed, and cefotaxime was administered intravenously (200mg/kg/day). Ultrasound of the chest and abdomen showed effusion without lung involvement and a splenic cyst (79mm×74mm) (Fig. 1). A follow-up ultrasound showed increased effusion, left basal pulmonary consolidation and elevated diaphragm, secondary to splenic cyst. Ampicillin-resistant Salmonella enterica serotype Enteritidis was isolated from a fecal culture. Pleural drainage fluid contained red blood cells 1440/mm3, leukocytes 29 610/mm3 (90% polynuclear), glucose 41mg/dl, protein 3.4g/dl and lactic acid 32mg/dl. Gram stain, culture, CRP and pneumococcal antigen were negative. The patient worsened unexpectedly, so a chest-abdomen ultrasound was performed, revealing an increase in cyst size. After contrast-enhanced abdominal computed tomography (CT), the splenic abscess was drained and Salmonella spp. (same type and sensitivity) were isolated from drainage fluid. Drainage was repeated due to abdominal pain and cyst enlargement. This time, the culture was negative and capsulectomy was scheduled. Antibiotic therapy was switched to meropenem (48mg/kg/8h). Progress was favorable, and minimal pleural thickening without effusion was seen on the chest-abdomen CT, while no images suggestive of cyst were seen on ultrasound. The initial prescription of ampicillin in our case is questionable, given the considerable rate of resistance (40% in our hospital). The early switch to cefotaxime, initiated due to radiological findings initially interpreted as pneumonia, may have prevented a poor outcome, but on the other hand, this erroneous interpretation complicated the diagnosis. Chest X-ray is a sensitive imaging technique for directing attention toward the left upper quadrant, but it lacks specificity for the diagnosis of splenic abscess. As a result, the pleural effusion observed is interpreted, as in this case, as a clinical sign of pneumonia, thus delaying the real diagnosis. Abdominal CT is the technique of choice in the case of suspected splenic abscess, and its use has improved detection of this disease. Incidence has also increased due to the greater prevalence of immunosuppressive states, producing more reports in recent series of fungal etiologies.3,4 In this respect, our case is uncommon, due to the lack of predisposing factors, such as immunosuppression or endocarditis. Conventional treatment is antibiotic therapy and total or partial splenectomy, although percutaneous drainage may be considered in patients with contraindications for surgery.5
Please cite this article as: González-Abad MJ, Alonso Sanz M. Condensación pulmonar versus absceso esplénico por Salmonella. Arch Bronconeumol. 2016;52:169–170.