Neurogenic tumors represent approximately 20% of all mediastinal neoplasms in adults.1 Anatomically, they can derive from the nerve sheath, the ganglion cells or from the paraganglion system. The majority are benign tumors and are located in the posterior mediastinum at the level of the paravertebral gutter, coming from the root of either an intercostal or sympathetic nerve.2 Only between 4% and 6% originate in the visceral compartment from the nerve sheaths of the vagus or phrenic nerves.3
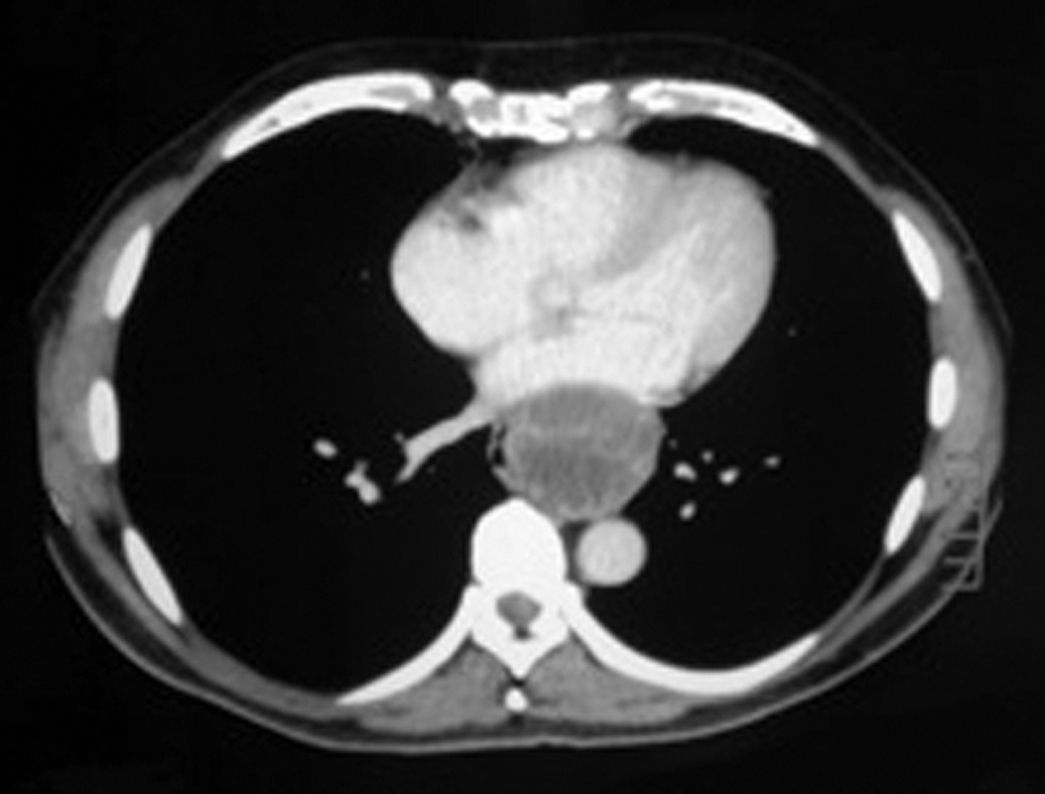
We present the case of a 53-year-old male with a personal history of HTN and right peripheral facial paralysis for the last 2 years. In the study for a possible myopathy, simple chest x-ray revealed a posterior mediastinal mass, and the patient was referred to our department. The study of the patent was completed with thoracic CT that confirmed a mass measuring 63×57mm that was hypodense, walled and localized in the posterior mediastinum (Fig. 1). It was causing compression and a displacement of the lumen of the lower third of the esophagus and of the posterior wall of the left auricle, compatible with a possible esophageal leiomyoma. Left posterior thoracotomy was carried out through the 7th intercostal space, finding a cystic, encapsulated tumor located in the pathway of the left vagus nerve. The lesion was extra-esophageal and was covered by the paraesophageal mediastinal pleura. It was completely resected after ligating the vascular pedicles and liberating the adherences over the esophagus. The histopathological report revealed a cystic tumor measuring 65×58mm that was unilocular and presented a classic biphasic pattern, alternating with areas of Antoni type A and type B of the benign schwannomas. Post-op presented no complications, and the patient was discharged on the third day after the intervention.
The patient currently continues to be asymptomatic and disease-free 26 months later.
Schwannomas are tumors of the nerve sheath originating in the nerve roots or the peripheral nerves.4 More often than not, they are located in the head, neck and extremities.1,2 They may also present within the thorax, originating in the sympathetic chain, spinal nerve roots, intercostal nerves, brachial plexus, phrenic nerve or vagus nerve.1,2 Schwannomas of the vagus nerve are located above all in on the left side,5 as in our case, as the nerve trunk is longer and wider.
They usually present no symptoms4 except for the compression of neighboring structures, frequently appearing as incidental radiological findings.3,4 The treatment of choice is surgical exeresis,2 which also allows for the diagnosis to be made. The approach may be either by means of thoracotomy or video-assisted thoracoscopy.2 The latter may be contraindicated in tumors larger than 6cm.5 In our case, we decided to perform an approach through a posterior thoracotomy in the 7th intercostal space due to the size of the lesion and the differential diagnosis with an esophageal leiomyoma-type tumor or gastrointestinal stromal tumor (GIST).
Complete exeresis of benign schwannomas is considered curative as recurrence is infrequent.
Although they are very rare, schwannomas of the vagus nerve should be included in the differential diagnosis of posterior mediastinal masses in close association with the esophagus, together with other mediastinal neurogenic tumors, lymphomas, mediastinal cystic lesions and esophageal tumors.
Please cite this article as: Muñoz PM, et al. Schwannoma del nervio vago intratorácico. Arch Bronconeumol. 2011;47:374–5.