Hypersensitivity pneumonitis (HP), or extrinsic allergic alveolitis, is a group of inflammatory lung diseases that usually affect the more peripheral airways and are induced immunologically after the reiterated inhalation of different materials, fundamentally organic substances and low-molecular-weight chemical compounds.1 Disorders similar to HP have been described in patients who have had massive exposure to nontuberculous mycobacteria (NTM), especially by inhaling them from hot water aerosol sources like saunas, etc. The NTM that has been described in practically all these cases is Mycobacterium avium-complex, although M. immunogenicum has also been reported.2
We present the case of a 29-year-old woman, originally from Colombia, who has been living in Spain for the last 4 years. The patient was working as a receptionist at a Spa. She had no toxic habits or personal medical/surgical history of interest. Prior to admittance, she had no history of asthma-type respiratory pathology or known tuberculosis contact. She came to our emergency department with symptoms of cough without expectoration and 39°C fever, and was diagnosed with bronchial hyperreactivity. She was prescribed bronchodilator treatment and was discharged. Two weeks later, she came to the emergency department once again due to sudden dyspnea when climbing stairs associated with a feeling of retrosternal oppression that increased with deep breathing and palpitations. During the patient interview, the patient commented that at her workplace, after renovations were done approximately one year before, a sort of niche was created in a wall, and pigeons had been nesting there.
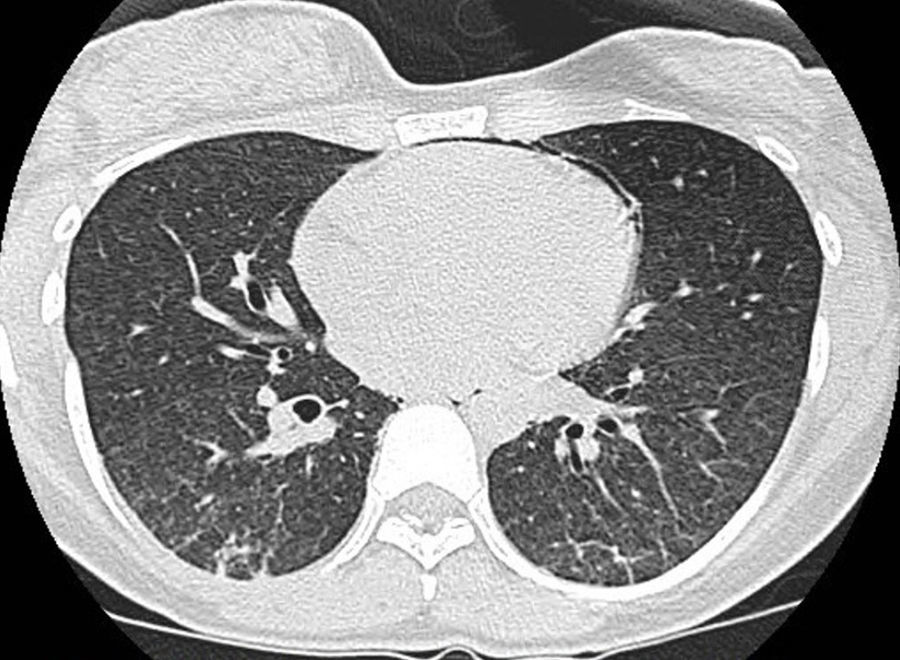
Upon physical examination, the patient presented no fever, tachycardia (140bpm), tachypnea (36 breaths per minute) and baseline oxygen saturation (breathing room air) of 91%. Lung auscultation showed preserved vesicular murmur with bibasilar crackles. Blood workup revealed normal ionogram, C-reactive protein 80g/dl, leukocytes 11430mm3 (90% neutrophils and 1.4% eosinophils), hemoglobin 12.4g/dl, hematocrits 36.4%, platelets 309000mm3. Baseline arterial blood gas analysis reported pH 7.44, pCO2 31mmHg, pO2 54mmHg, CO3H 21.1mmol/L. Chest radiography showed a bilateral micronodular pattern in both lung bases associated with mild fissure thickening. Diagnostic bronchoscopy demonstrated no endobronchial lesions, and samples were taken from the bronchoalveolar lavage and aspirate as well as a transbronchial biopsy. In the lavage, a moderate number of lymphocytes were observed along with polymorphonuclear cells. No eosinophils were observed. The biopsy showed fragments of lung parenchyma with isolated non-necrotizing epithelioid granulomas and isolated giant cells situated at the septum. Histochemical stains for detection of acid-fast bacilli (Kin-Youn) were negative. The bronchial aspirate was also negative for malignancy. In three sputum culture samples, Mycobacterium avium was isolated and the pigeon precipitin study was negative. Thoracic tomography (HRCT) showed an interstitial pattern with diffuse bilateral centrilobular nodules, together with images of airway consolidation in the sloping parts of both bases, probably related with atelectasis, as well as pneumomediastinum related with the transbronchial biopsy. No mediastinal or axial pathologic lymphadenopathies were observed (see Fig. 1).
Given the diagnostic suspicion for hypersensitivity pneumonitis, treatment was initiated with corticosteroids (0.5mg/kg), and the patient presented improved symptoms and gas exchange, with baseline saturation at discharge of 97%. The follow-up X-ray 7 days later also showed very favorable evolution, both of the pneumomediastinum (hardly visible), as well as the interstitial pattern, which was only present in the lung bases.
Hypersensitivity pneumonitis due to exposure to Mycobacterium avium is an emerging disease caused by exposure to whirlpool bathwater contaminated by said bacteria (“hot tub lung”, “Jacuzzi lung”). Several cases have been reported since 1997.3–5 These patients have been treated with antimycobacterial and/or corticosteroid therapy, although some patients improve by simply avoiding contact with the source of exposure. There has been continuous debate about the optimal management of this pathology given that the need for antimycobacterial treatment is still controversial.5 In 2005, Hanak et al. carried out a retrospective review of 21 patients diagnosed with “hot tub lung” at a reference center in a 7-year period in order to analyze the characteristics and clinical evolution of these patients. The results of this study suggest that the entity behaves as a hypersensitivity pneumonitis more than as a mycobacterial infection, and therefore treatment with antimycobacterial drugs may not be essential.5
The patient's symptoms led us to consider the possibility of HP, although it was not very clear if it was secondary to exposure to pigeons. Given the improvement with corticosteroid therapy, we decided to send the patient home even though the results for precipitins and mycobacteria were pending. Once the diagnosis was confirmed, the Public Health Department was informed and the spa where the patient worked was closed.
Please cite this article as: Terrero Jiménez BM, et al. Neumonitis por hipersensibilidad por exposición a Mycobacterium avium. Arch Bronconeumol. 2013;49:173–4.