Introduction
Lung cancer remains, at the beginning of the 21st century, the tumor that causes the most deaths in developed countries. The difficulty in diagnosing lung cancer lies in the fact that symptoms usually appear late in the course of the disease and for that reason up to 80% of patients present at inoperable stages.1-3
In recent years much has been published on new methods of diagnostic imaging, bronchoscopy, genetic markers, and so on in order to achieve earlier management of lung cancer.4-7 While these undeniably represent significant advances, another practical problem has received less attention--the reasons for delays in consulting for suspicious symptoms and delays in diagnosis and treatment.
Several international and Spanish studies have revealed the inadmissible delays that exist in the diagnosis of this fatal disease.8-11 Our work group12 also observed, in a preliminary prospective study of 56 patients, excessive diagnostic delays from the onset of suspicious symptoms.
How much responsibility for this is attributable to the organization of the health care system? How much to lack of health awareness on the part of patients or of training given to doctors?
If we are not able to answer or at least consider these questions, we can do little to look for possible solutions.
The aim of our study was to analyze the epidemiological and clinical factors of health care that might have affected diagnostic delays. These aspects received little attention in the studies previously cited and we believe they are important in answering the above-mentioned questions.
Patients and Methods
Ours was a prospective study carried out during the period from January 1, 2000 to December 31, 2001. All the patients admitted to our service for suspected diagnosis of pulmonary neoplasia were initially included. During follow-up all patients for whom the TNM characterization or other findings of pathology had not been completed, those for whom the final diagnosis was not primary pulmonary neoplasia, and those who had not been admitted to hospital were excluded from the study. Of the 150 patients identified and included, 37 were excluded for the above-mentioned reasons, and only 113 were finally accepted.
A data-gathering protocol was designed which included:
--Sociodemographic information on patients: sex, age, place of residence (rural or urban) number of people living with them, availability of medical services in their locality, profession, their own or family history of tumors, smoking history, and level of education (no schooling, primary, secondary or university studies).
--Medical aspects: Comorbidity (smoking-related diseases were recorded), medical services in the habitual place of residence (primary care physician, health center or hospital), patient's first symptom (of those considered possibly indicative of tumoral disease), symptom leading to consultation (if different from first symptom), medical service consulted (primary care physician, emergency room or pulmonologist), and the action taken by the health care professional. Finally, we recorded data on the total number of consultations and doctors seen from the onset of symptoms to assessment of the patient by the respiratory medicine service.
--Data collected during the hospital stay: Time taken to order, perform and obtain results of computed tomography (CT), findings of fiberoptic bronchoscopy and the pathologist's diagnosis. Total length of hospital stay was also recorded.
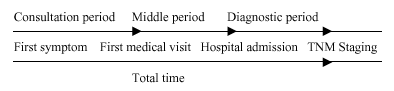
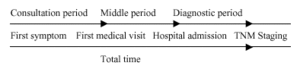
We studied the following diagnostic time periods: consultation, which covers the interval from first pathological symptoms related to the presence of pulmonary neoplasia to first consultation with a medical professional; middle period, the interval between first medical visit and hospital admission; diagnostic, the interval between first consultation in the respiratory medicine service and complete TNM staging and the pathologist's diagnosis; and finally, total time, which is the sum of the previous time periods.
The statistical analysis was done by means of a database created for the purpose in SPSS software version 9. Values are expressed as means (SD) and 95% confidence intervals (CI).
In addition to the descriptive analysis, parametric (Student t and one-way analysis of variance) and nonparametric tests (in the case of small samples or nonnormal distributions) were done. A P value less than .05 was considered significant.
The TNM staging was done according to the guidelines of the Spanish Society of Pulmonology and Thoracic Surgery (SEPAR).13
Results
One hundred thirteen patients with a mean age of 65(10.8) years (range, 36-90), 103 men and 10 women, were included in the study. Ninety-three percent were or had been smokers and 7% nonsmokers. The majority (57%) lived in rural areas. With respect to educational level, 65% had completed basic, 14% higher secondary, and only 7% university studies. Forty-five percent lived at home with 1 other person, 21% with 2 and 12% lived alone. Ten percent had a medical history of tumors and 5% a family history of neoplasia. Only 8% were in high-risk professions for lung cancer.
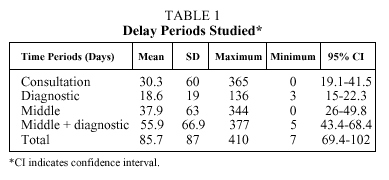
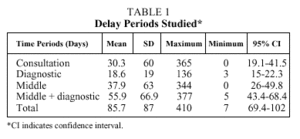
The mean time periods, expressed in days, are shown in Table 1. The only delay related to place of residence occurred in the consultation period, which was longer in urban (39[82.3] days) than in rural (23.7[35] days) areas (P=.01).
For patients with a medical history of neoplasia, the diagnostic time period was longer: 21.8(17) days compared to 13(6) days for patients with no such history (P<.001). There were no differences in the other time periods.
With respect to age, we found no statistically significant differences in the diagnostic time periods.
Nor did we find significant differences with respect to educational level (no schooling, primary, secondary, or university studies), or to smoking history.
As for access to health care, 39% had been able to go to a primary care physician's office, 10% to a clinic, and 51% to a hospital. No significant differences in delays were observed.
Fifty percent of the patients were seen by 2 doctors during the diagnostic process, 22% by 3, 20% by 1, and 7% by 4 or more. As to the number of doctor's visits, 44% made 2 or 3, 17% only 1, and 12 as many as 6.
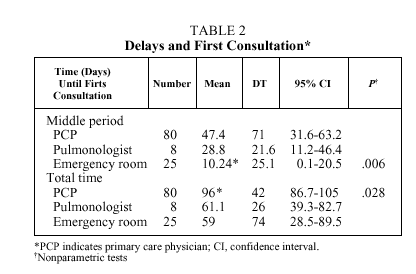
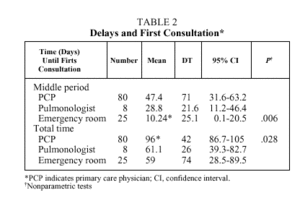
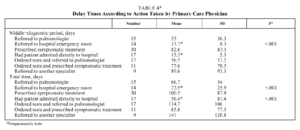
With regard to the type of doctor first consulted, 72% went to their assigned primary care physician, 6% to a pulmonologist, and 22% to a hospital emergency room. Delays were shorter when the first consultation was in a hospital emergency room, and the total time period longer when the initial visit was to the assigned primary care physician. The differences were statistically significant in both instances (Table 2). No differences were observed in the consultation or diagnostic time periods.
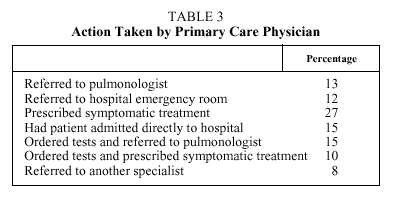
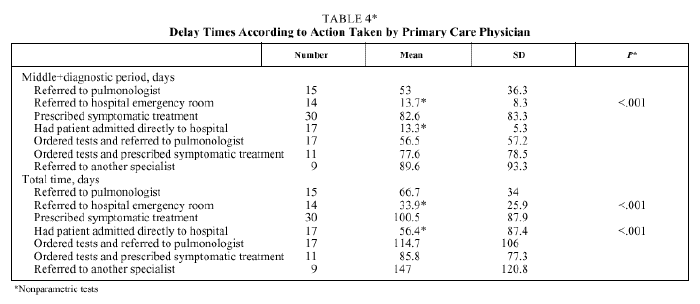
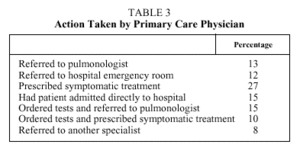
The action taken by the primary care physician is reflected in Tables 3 and 4. The middle and total time periods were significantly shorter when patients were referred to the emergency room and when they were directly admitted to hospital (Table 4).
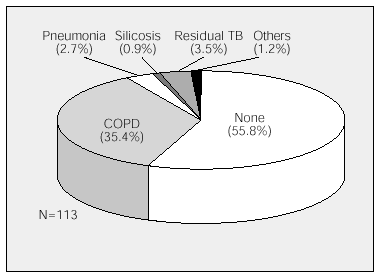
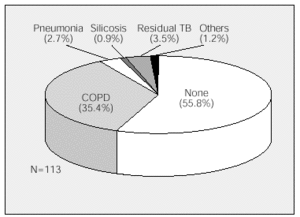
Respiratory comorbidity is shown in the figure. We found no differences in delays among patients with the various associated diseases.
Figure. Respiratory comorbidity associated with lung cancer. TB indicates tuberculosis; COPD, chronic obstructive pulmonary disease.
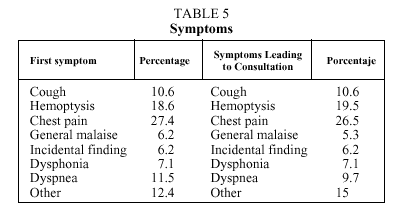
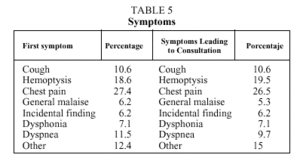
The patients' first symptoms and those that led them to seek medical advice are shown in Table 5. No relation between these symptoms and delay periods was found.
The procedures used for conclusive diagnosis were fiberoptic bronchoscopy in 51% of the cases, transthoracic needle aspiration in 36%, sputum cytology in 3%, and surgical biopsy and thoracocentesis in 2.7% each. We found no relation between the different diagnostic procedures used and diagnostic time period.
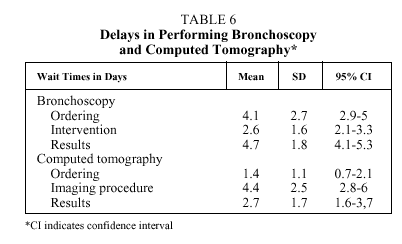
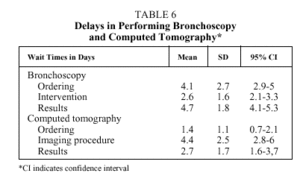
Delays in ordering, performing and obtaining the results of fiberoptic bronchoscopy and CT are shown in Table 6.
The most frequent cytologic or histologic types were: epidermoid (49.5%), adenocarcinoma (26%), and microcytic (13.8%).
Cases of microcytic lung cancer were included in TNM staging. Of the total study population, 25.7% were presumably operable (from I-A to III-A) and 74.3% inoperable. Twenty-four percent of the patients were referred for surgery and 18% were operated on (with, in some cases, preoperative adjuvant chemotherapy); the rest were referred to the oncology unit.
Discussion
Although we agree with authors who believe that hospitalization of lung cancer patients is often unjustified,10 we nevertheless feel that excessive delays in performing CT severely compromised the treatment of our outpatients during the period studied.
The variables associated with longer or shorter delays coincided approximately with those of a classic study on diagnostic delays in esophageal cancer.14
The demographic characteristics (age, sex, smoking history, and place of residence) obtained in the sample of patients studied by our pulmonology service are similar to those obtained in the study of the incidence of bronchogenic carcinoma in our autonomous Spanish community, Catalonia.3,15
The delay times we found, shown in Table 1, were as long as those published in a British study by Dische et al,16 in which the diagnostic delay from the first symptom to histological diagnosis was 13 weeks. The same authors considered delays longer than 8 weeks between the first medical consultation and thoracotomy unacceptable. The authors of another prospective study8 also found the period from the first symptom to diagnosis excessively long (more than 90 days in 50% of the cases). In our case, the mean time was 55.9 days, which, added to the waiting period for thoracic intervention (data not considered in our study), would be longer than the unacceptable 8 weeks mentioned above. In the study carried out by the Bronchogenic Carcinoma Cooperative Group of SEPAR,10 the mean total delay between diagnosis and the thoracotomy was only 45(34) days. This study did not examine the time elapsing between the first symptom and diagnosis.
The fact that the consultation period was shorter in patients living in rural rather than urban areas (23.7 compared to 39 days) may be attributable to the greater accessibility of the primary care physician in these areas.
When the first consultation was in the hospital emergency room, the middle period was significantly reduced by about 34 days compared to that period for patients who first consulted a primary care physician, and by only 19 days compared to the time for patients who first consulted a pulmonologist (Table 2).
The longer delay in patients who first visited primary care physicians may be due to the fact that the doctors' decision was, in 52% of the cases, to prescribe symptomatic treatment, or order tests or radiographs (Table 3).
Delays were affected by primary care physicians' decisions. Thus, the middle, diagnostic and total time periods were significantly shorter when physicians elected to refer patients to the hospital emergency room or when the patient was admitted (Table 4).
Taking consultation with a pulmonologist as a reference, the mean reduction in total time was about 40 days if the patient was referred to the emergency room and only 10 days if directly admitted to hospital. The increase in total time was greatest if the patient was referred to another specialist (about 80 days) or was first given previous symptomatic treatment (about 34 days). The exact figures are given in Table 4.
A possible interpretation of these data is that it is difficult to reduce the middle period when, as is the case in our setting, there is a certain delay in pulmonology services.
These delays could be made shorter by introducing organizational changes in the health care system, such as rapid response respiratory care services, which represent an important advance toward early diagnosis. Positive experiences have been reported from other autonomous communities in Spain that have opened emergency outpatient clinics based on the principle of cooperation between primary and specialized care providers.17
More recently, these one-stop clinics or rapid response services for diagnosing lung cancer have spread to other autonomous communities in Spain.18-20 The results published indicate a marked reduction in the diagnostic delays between medical assessment and treatment. The delays between onset of symptoms and first medical consultation, probably connected with the natural history of the disease and the patient's own level of health awareness, still need to be shortened.
It is still unclear what effect, if any, this would have on earlier presentation of patients with lung cancer and consequent reduction in the percentage of inoperable cases, which in our setting is currently 74%.
Fifty percent of our patients were seen by 2 doctors (in general, a primary care physician and a pulmonologist), somewhat fewer than in the study of de Silva et al,9 where the average was 3 or 4 doctors. As 72% of first visits were to primary care physicians, their approaches and training are of prime importance.
Respiratory comorbidity was present in 44% of our sample, with chronic obstructive pulmonary disease predominating. This may be the reason why the most frequent symptoms suggestive of possible lung cancer (coughing, hemoptysis, and chest pain) were not associated with a longer or shorter diagnostic delay.
Usual presenting symptoms are those mentioned above, together with shortness of breath or general malaise. These may either be a first symptom or the symptom leading to consultation.6,11
We only studied the delays in 2 diagnostic tests, fiberoptic bronchoscopy and CT, which were performed in all cases. The rest of the tests, (laboratory, radiographic, spirometric, etc.) did not constitute a cause of delay, as they are performed routinely and simultaneously.
Once the patient had been admitted, it took 7.4(2.3) days from the time fiberoptic bronchoscopy was ordered until it was performed and a histological diagnosis obtained, and an additional 7.1(3.2) days for CT (excluding cases needing transthoracic needle aspiration). The breakdown of test timing is shown in Table 6. These middle period delays, with respect to bronchoscopy, are shorter than the ones published by Carrasquer et al11 (10 days) and by López Encuentra et al10 (9.5 days) in Spain, and also shorter than those obtained in other European studies (14 days in the British study of Billing and Wells8).
In conclusion, delays in lung cancer diagnosis are long. The attitudes of primary care physicians and their relations with specialized care providers can be important for reducing them, leading to earlier diagnosis of lung cancer and perhaps an increase in the number of operable cases.
Acknowledgments
To the lung surgery service of the Hospital Universitario de Salamanca.
Correspondence: Dr. J.M. González Ruiz.
Avda. de Salamanca, 268, 3.º C. 37005 Salamanca. España.
E-mail: jmgonzru@usal.es
Manuscript received January 22, 2003.
Accepted for publication May 13, 2003.