Our patient was a 74-year-old woman admitted for arteritic optic neuropathy. She had a history of pulmonary tuberculosis in her youth, chronic Pseudomonas aeruginosa bronchial infection treated with inhaled colistin, and rheumatoid arthritis initially treated with methotrexate, which was discontinued when usual interstitial pneumonia was detected. Treatment began with azathioprine, adalimumab, and rituximab, but was discontinued given a lack of response. She was not currently receiving any specific treatment.
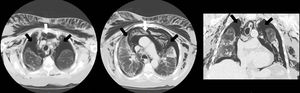
During admission after an episode of cough, she presented dyspnea, subcutaneous emphysema, and bitonal voice; pneumothorax was suspected and chest X-rays and CT scans were requested (Fig. 1).
The patient was treated by placement of a pleural drain in the left hemithorax and oxygen therapy.
Both bilateral spontaneous pneumothorax and spontaneous pneumomediastinum are very rare entities seen mainly in patients with underlying lung disease.1 Only a small number of cases is associated with rheumatoid arthritis.
Spontaneous bilateral pneumothorax is treated by placement of pleural drains when significant, while treatment of pneumomediastinum is conservative. In high-risk patients such as those with advanced interstitial disease, early use of inhaled oxygen at high concentrations may result in rapid resolution, with no recurrence at 6 months of follow-up.2
Please cite this article as: Carrasco CCM, Asuero Llanes A, Alfageme Michavila I. Neumotórax bilateral espontáneo secundario y neumomediastino en paciente con EPID por artritis reumatoide. Arch Bronconeumol. 2020;56:665.