Foreign bodies impaled in the chest are rare and generate a dramatic situation for the patient, the relatives and the trauma team. The standard approach in these cases has always been open thoractomy.1 Video-assisted thoracoscopy surgery (VATS) is a relatively recent indication in the management of impaled foreign bodies.
We report 2 cases where VATS was used in the management of chest impalement with knives.
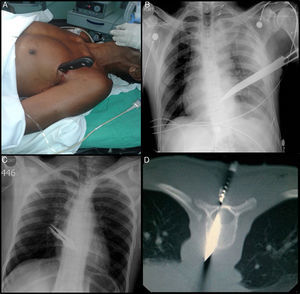
In the first case, a 62-year-old man was stabbed in the left thorax with a kitchen knife. The knife entered the thorax at the 4th intercostal space at the level of the anterior axillary line (Fig. 1A). The patient was hemodynamically stable. Chest radiograph showed left hemothorax and the knife could be visualized above the cardiac silhouette (Fig. 1B). He was transferred to the operating room and examined by thoracoscopy, which showed that the knife had penetrated the upper lobe of the lung. The hemothorax was aspirated and the knife was extracted under direct vision. The pulmonary laceration was sutured by thoracoscopically. In the second case, a young man aged 18 years presented with a serrated knife impaled at the level of the 9th thoracic vertebra. His vital signs on arrival at hospital were: blood pressure: 129/57mmHg, heart rate: 65bpm, and breathing rate: 20breaths/min. Neurological examination showed a complete medullary lesion below the wound. No hemothorax or pneumothorax were seen on chest radiograph (Fig. 1C) and computed tomography of the spine showed that the knife had sectioned the spinal cord (Fig. 1D). Orotracheal intubation was achieved by positioning the patient between 2 gurneys in order to place him in a supine position. Thoracoscopic examination revealed a posterior mediastinal hematoma, so the procedure had to be switched to thoracotomy. An injury was revealed in the thoracic aorta that could be repaired with polypropelene suturing. In both cases, the post-operative period was incident-free.
VATS in chest injury was initially indicated for diagnostic purposes and for management of coagulated hemothorax. Abolhoda et al.2 used it to rule out perforated diaphragm and to successfully treat several cases of post-traumatic retained hemothorax. Lang-Lazdunski et al.3 extended the indications of thoracoscopy in chest trauma to include persistent hemothorax, intrathoracic foreign body, post-traumatic empyema, and post-traumatic chylothorax. As surgeons gain more experience and technology improves, the treatment of more complex injuries has become possible. Few reports are available on VATS management of foreign bodies impaled in the chest, but we agree with Isenburg et al.4 in that these patients must be hemodynamically stable before a thoracoscopic approach can be attempted; otherwise, open thoracotomy must be initiated directly.
In brief, the thoracoscopic management of foreign bodies impaled in the chest is a safe and effective option for the hemodynamically stable patient. VATS has specific advantages. It is a minimally invasive diagnostic and therapeutic procedure. In addition to establishing the severity of the lesions, the surgeon can employ it to identify potential complications for removal of the foreign body and to repair the different wounds.
FundingThe authors received financial support from the National Secretariat of Science, Technology and Innovation (SENACYT), a governmental institution for the promotion of research.
Please cite this article as: Andrade-Alegre R, Donoso N, El-Achtar O. Videotoracoscopia para el diagnóstico y tratamiento de los empalamientos por cuchillo en el tórax. Arch Bronconeumol. 2016;52:394–395.