Primary pulmonary lymphoma accounts for 3%–4% of extranodal non-Hodgkin's lymphoma, less than 1% of non-Hodgkin's lymphoma, and only 0.5%–1% of primary pulmonary cancers.1 The most common presentation is bilateral pulmonary infiltrate, whether in the form of nodules or a cavitated mass. Other less common presentations are air bronchogram, ground glass areas, pleural effusion, and atelectasis.2,3 However, a unilateral presentation is rare. Diffuse large B-cell lymphoma (DLBCL) accounts for approximately 15% of cases of non-Hodgkin's lymphomas.1
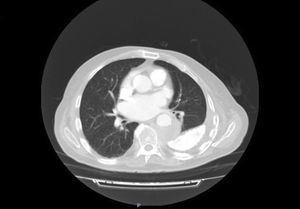
We report the case of a 75-year-old man who consulted due to asthenia, anorexia, and weight loss of about 10kg in 3 months, accompanied by pleuritic pain in the left hemithorax and intermittent dyspnea. He also reported a perforating injury in the left hemithorax that occurred several years ago. No toxic habits or exposure to physical or chemical agents were recorded, and personal history included arterial hypertension, type 2 diabetes mellitus, ischemic heart disease, and atrial fibrillation with permanent anticoagulation. The only finding of interest on examination was cachexia with hypoventilation in both lung bases and basal oxygen saturation of 98%. A raised left hemidiaphragm associated with a basal area of pulmonary consolidation and extensive pleural thickening, consistent with diffuse pleural fibrosis, were observed on chest X-ray. Clinical laboratory tests revealed normocytic anemia consistent with chronic disorders, neutrophilia without leukocytosis, slightly elevated beta-2-microglobulin, and hypoalbuminemia with no evidence of clonal spikes. Chest computed tomography (CT) revealed a tumor measuring 5.3×9.6cm, adjacent to the descending thoracic aorta, with contrast medium uptake, apparently in contact with the left lower lobar bronchus, associated with an extensive area of pleural calcification. No associated lymphadenopathies were observed (Fig. 1). The remaining exploratory studies were normal. A positron emission tomography/CT (PET/CT) was performed in order to determine the nature of the lesion and to complete the study. This procedure revealed increased metabolic activity in the lesion, with an increased cellular proliferation rate, and possible infiltration of the D9 vertebra and posterolateral region of the chest wall. Fiberoptic bronchoscopy was ruled out, as the lesion would have been inaccessible with this technique. CT-guided core needle biopsy was performed, and histological results showed Epstein–Barr virus (EBV) positive DLBCL-NOS. The patient was referred to the medical oncology clinic to plan treatment and follow-up.
Primary pulmonary lymphomas (PPL) are very rare, and account for less than 1% of cases of pulmonary neoplasms. PPLs are understood to be a disease exclusively involving the lung, with no evidence of extrathoracic, mediastinal, lymphatic or bone marrow involvement.4 Presentation tends to be bilateral, usually in the form of masses or nodules that generally cavitate (around 50% of cases), and less frequently as ground glass areas, or with pleural involvement, air bronchogram, reticular images, or lobar atelectasis.3 DLBCL is the most common form of non-Hodgkin's lymphoma (NHL), and accounts for 15%-25% of cases, depending on the series.1,4 This type of lymphoma constitutes a heterogeneous group with its own clinical, morphological, genetic and biological signature. The most common extranodal site is the gastrointestinal tract. It is diagnosed more frequently in men over 60 years of age, although it has been reported in patients younger than 30. Half of these tumors are diagnosed in a disseminated stage, and the other half as localized disease, in other words, contained within the area of 1 radiation field. DLBCL is locally very invasive. EBV-positive DLBCL is a specific variant that was added to the World Health Organization classification system in 2016. It can occur at any age, and is generally diagnosed in patients with no history of immunodeficiency or other lymphomas.1 This entity can overlap with lymphomatoid granulomatosis, the difference being in the appearance of EBV-positive B cells (which are scant otherwise). Our case is unusual due to the very rare manifestation of EBV-positive DLBCL as primary pulmonary lymphoma, along with the unilateral, non-cavitated pulmonary consolidation. We were unable to establish any association with the residual area of chronic pleural calcification, despite an extensive review of the literature.
Please cite this article as: Delgado Torralbo JA, García Gómez LC, Sánchez Varilla JM. Infiltrado pulmonar unilateral: una forma rara de presentación de un linfoma pulmonar primario. Arch Bronconeumol. 2018;54:103–104.