Thrombotic microangiopathy (TMA) is a rare complication associated with the use of calcineurin inhibitors in lung transplantation, irrespective of the underlying disease of the graft recipient. It usually occurs in incomplete forms, complicating and delaying diagnosis until damage is already irreversible. It is unrelated to time from transplantation and often presents with concomitant infection, which tends to confound diagnosis. The cases discussed here have a common causative agent and all present with concomitant infection. Treatment recommendations have changed in recent years with the introduction of plasmapheresis or, more recently, the availability of the antibody eculizumab. Notwithstanding, the most cost-effective measure is withdrawal or switching of the calcineurin inhibitor. TMA is an underdiagnosed clinical entity that should be considered in the management of transplantation patients.
La microangiopatía trombótica (MAT) es una complicación infrecuente asociada a los anticalcineurínicos en el trasplante pulmonar, independiente de la enfermedad de base de los pacientes trasplantados. Habitualmente se presenta como formas incompletas, lo que dificulta el diagnóstico, que suele ser tardío, provocando irreversibilidad de las lesiones. Es independiente del tiempo de trasplante y en muchos casos existe infección concomitante, lo que tiende a ocultar el diagnóstico. Los casos presentados comparten el agente causal y la presencia de infección concomitante. El tratamiento ha variado en los últimos años, recomendándose la plasmaféresis o, más recientemente, el anticuerpo eculizumab. No obstante, la retirada o cambio del anticalcineurínico causante es la medida más coste-efectiva. La MAT podría tratarse de una entidad infradiagnosticada a tener en cuenta en pacientes trasplantados.
Transplant-associated thrombotic microangiopathy (TMA) rarely presents with all 5 of the typical signs–hemolytic anemia, arteriole and capillary damage, thrombocytopenia, fever and neurological disorders–so clinical suspicion is essential for an early diagnosis.1 There are many predisposing factors for TMA in transplant patients. In addition to infections, calcineurin inhibitors have been identified as causative agents in most cases, and withdrawal of these drugs, along with other measures, has been shown to be the most effective approach.2,3 We report 3 cases of TMA associated with tacrolimus triggered by an infectious process.
Case 1A 56-year-old man, a single-lung transplant recipient 6 years previously due to emphysema, was admitted due to Nocardia myositis that had formed an abscess in his right leg. Initial post-transplant immune suppressive treatment had included tacrolimus, mofetil mycophenolate and corticosteroids. He presented deteriorating renal function, with creatinine levels of 7.92mg/dl compared with baseline admission levels of 3.26mg/dl. He developed anemia, with hemoglobin 7.92g/dl (12.5g/dl on admission), and thrombocytopenia 72000/μl. LDH was 794U/l. The myositis abscess was successfully treated, but there was no improvement in renal function, anemia or thrombocytopenia, and schistocytes were detected in peripheral blood. In view of suspected TMA, bone marrow aspirate was obtained, showing predominant erythroid cell series, with fragmented forms suggestive of microangiopathic anemia. Tacrolimus was thought to be the probable cause, so it was switched to everolimus. In subsequent tests, creatinine figures fell to 5.5mg/dl in 1 week and returned to baseline in following check-ups. Platelets and hemoglobin levels recovered gradually (Table 1).
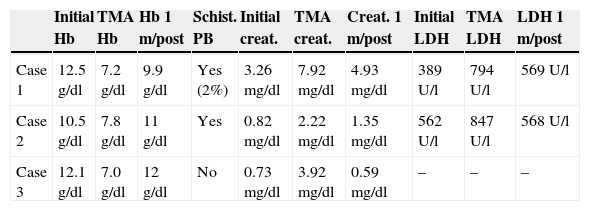
Summary of Changes in Hemoglobin, Creatinine and LDH in the 3 Cases.
| Initial Hb | TMA Hb | Hb 1m/post | Schist. PB | Initial creat. | TMA creat. | Creat. 1m/post | Initial LDH | TMA LDH | LDH 1m/post | |
|---|---|---|---|---|---|---|---|---|---|---|
| Case 1 | 12.5g/dl | 7.2g/dl | 9.9g/dl | Yes (2%) | 3.26mg/dl | 7.92mg/dl | 4.93mg/dl | 389U/l | 794U/l | 569U/l |
| Case 2 | 10.5g/dl | 7.8g/dl | 11g/dl | Yes | 0.82mg/dl | 2.22mg/dl | 1.35mg/dl | 562U/l | 847U/l | 568U/l |
| Case 3 | 12.1g/dl | 7.0g/dl | 12g/dl | No | 0.73mg/dl | 3.92mg/dl | 0.59mg/dl | – | – | – |
Creat.: creatinine; Schist. PB: schistocytes in peripheral blood; Hb: hemoglobin; LDH: lactate dehydrogenate; TMA: thrombotic microangiopathy; 1m/post: one month after diagnosis of thrombotic microangiopathy.
A 61-year-old woman, a double-lung transplant recipient 6 months previously for idiopathic pulmonary fibrosis, was admitted due to left lower lobe pneumonia, weakness and deteriorating renal function. Creatinine levels, previously normal, had risen to 2.22mg/dl. The patient also presented anemia 7.8g/dl (initially 10.5g/dl) and thrombocytopenia 68000/μl, so a platelet transfusion was administered, but the thrombocytopenia could not be permanently reversed. Intensive immunosuppressive therapy continued with tacrolimus, mycophenolate and corticosteroids. During admission, she received antibiotic and antifungal treatment. Radiological improvement was seen, but altered renal function, anemia and LDH of 847U/l persisted. A morphological study of the blood revealed some very isolated schistocytes and low haptoglobin levels, so the calcineurin inhibitor tacrolimus was switched to everolimus, while the other immunosuppressive agents were continued unchanged. This led to a progressive fall in LDH, platelets normalized and creatinine levels fell to 1.35mg/dl within 1 week (Table 1). Hemoglobin stabilized at 11.0g/dl.
Case 3A 21-year-old woman had received a double-lung transplant 4 months previously for cystic fibrosis. She was receiving immunosuppressive therapy with tacrolimus, mofetil mycophenolate and corticosteroids. The patient was admitted with a febrile syndrome and an abscess in the area of the lower jaw. Candida glabrata was isolated from the abscess, but there was no hematogenous spread. Creatinine levels deteriorated, falling to 3.92mg/dl (0.73mg/dl on admission), hematocrit fell to 22.6% and thrombocytopenia to 18000/μl, causing repeated epistaxis. A platelet transfusion was administered but the situation could not be completely reversed. The abscess was successfully treated, but no improvements were found on clinical laboratory results, with persistent altered renal function, anemia, low-grade fever and low haptoglobin levels, suggestive of hemolysis. Tacrolimus was switched to everolimus, and the dose of corticosteroids was increased, leading to gradual return of creatinine levels to normal (Table 1). Hemoglobin rose to 11.5mg/dl and platelets to 145000/μl.
DiscussionTacrolimus is a metabolite extracted from the fungus Streptomyces tsukubaensis. It is a potent immunosuppressive agent widely used in transplant procedures. Tacrolimus-associated TMA is a rare, but potentially fatal, complication in solid organ and bone marrow transplantation, with an estimated incidence of 1.0%–4.7%.1,3 Early diagnosis is essential for improving treatment outcomes, but is difficult to achieve due to the existence, on occasions, of previous chronic renal failure (CRF) secondary to calcineurin inhibition. A definitive diagnosis is obtained from the renal biopsy finding of thrombi in the glomerular capillary loops. Treatment of drug-associated TMA is not well defined.2 Recommendations in the literature are conventionally based on switching the causative medication to sirolimus, everolimus or cyclosporin. If diagnosis is early, effective treatment is available, for example, the antibody eculizumab, or plasmapheresis.3,4 No cases of tacrolimus-associated TMA in lung transplant have been published in the Spanish literature, and few have been reported in the international literature.5 However, this entity may be underdiagnosed, and it should be considered in transplant patients receiving calcineurin inhibitors with deteriorating renal function and unexplained anemia. In our opinion, a kidney biopsy can be avoided if schistocytes are observed in peripheral blood along with low serum haptoglobin levels.
Conflict of InterestsThe authors declare they have no conflict of interests.
We thank Dr. Pilar Morales for her help.
Please cite this article as: Reig Mezquida JP, Solé Jover A, Ansótegui Barrera E, Escrivá Peiró J, Pastor Colom MD, Pastor Guillem J. Microangiopatía trombótica asociada a tacrolimus en trasplante pulmonar. Arch Bronconeumol. 2015;51:e23–e24.