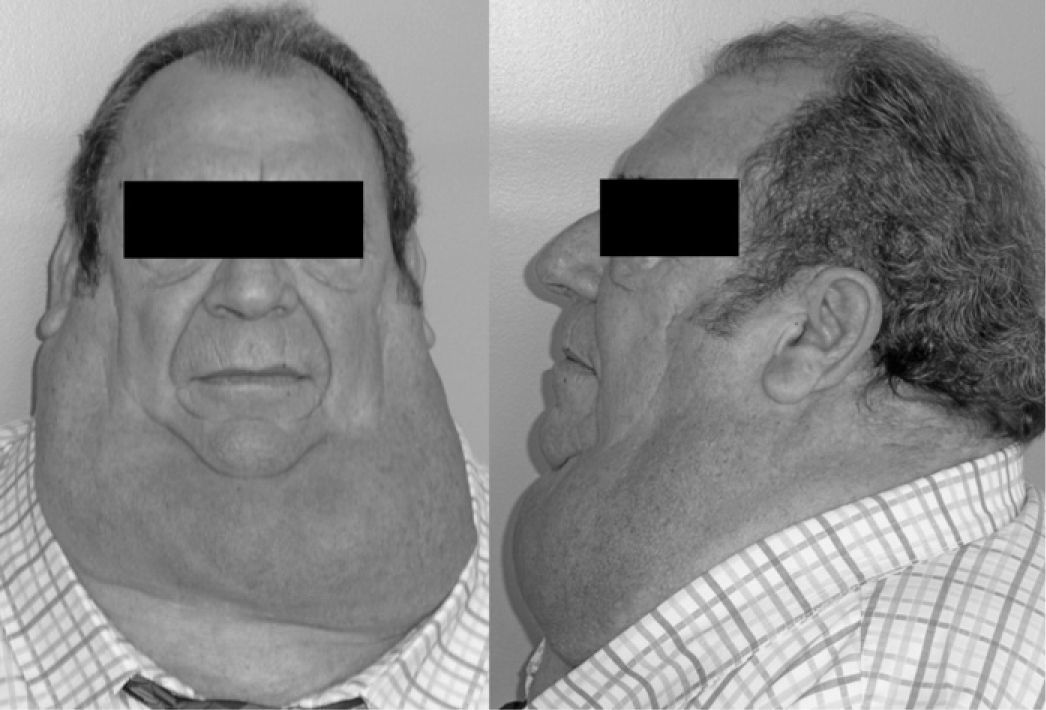
We believe that the readers of your journal will find it interesting the association of sleep apnea-hypopnea syndrome (SAHS) with a rare disease such as multiple symmetric lipomatosis (MSL), Madelung's or Launois–Bensaude syndrome. Said association has been reported in several publications in recent years, and we ourselves have witnessed this combination of diseases in one of our patients (Fig. 1). MSL is an uncommon disease of unknown etiology that is characterized by the symmetrical accumulation of fat in the form of non-encapsulated subcutaneous lipomas in different locations, although especially in the neck and shoulders.1,2 It is most frequent in males between the third and fifth decades of life, and it is frequently associated with alcoholism, chronic hepatopathy and neuropathy. It sometimes causes symptoms caused by the compression of neighboring structures such as the larynx. It can be associated with metabolic diseases and with atherogenic risk factors. Given the therapeutic implications, it should be differentiated from other rare adipose disorders. Diagnosis is usually symptoms-based, and when in doubt either computed tomography (CT) or magnetic resonance imaging (MRI) can be of help. MSL is a progressive disease with an infiltrating behavior. Diet control, alcohol abstinence and lymphatic drainage are recommended. In some cases, surgical reduction of the fat masses is the only treatment that may be effective and is aimed at improving esthetic and psychological consequences as well as treating airway or digestive tract obstruction, if necessary.
Very few cases have been reported of MSL associated with SAHS.2–6 The presence of large fatty deposits in the cervical area would contribute to the narrowing of the upper airway and could interfere with the normal function of the pharyngeal muscles during sleep, favoring the appearance of SAHS. The frequent association of alcoholism and obesity would likewise increase the risk for SAHS. The diagnosis and treatment of SAHS in patients with MSL is especially important due to the increased risk for cardiovascular and metabolic diseases when both diseases are associated. Although cases have been published in which SAHS has improved after surgical treatment of MSL, when we take into account the limited long-term effectiveness of this therapeutic option and the success of continuous positive airway pressure (CPAP) treatment in patients with MSL who present SAHS, it seems reasonable to indicate CPAP as a treatment of choice (together with standard diet and hygiene measures) as long as surgery is not indicated for another reason.
In conclusion, in patients diagnosed with MSL, SAHS should be suspected if there are symptoms indicating it, and CPAP treatment should be offered due to the good results obtained to date in published cases.
Conflict of InterestsThe authors declare having no conflict of interests.
Esteban Júlvez L, et al. Síndrome de apnea-hipopnea del sueño y lipomatosis simétrica múltiple. Arch Bronco-neumol. 2013;49:86–7.