The aim of this study was to determine the prevalence of venous thromboembolism (VTE) after elective thoracic surgery in patients receiving antithrombotic prophylaxis, and to evaluate the risk of pulmonary embolism (PE) after lung resection.
Patients and methodsA descriptive, cross-sectional, retrospective study was designed. A total of 6004 patients were included. All patients underwent elective thoracic surgery. Prophylactic antithrombotic therapy was standardized in all cases. Patients were divided into four groups (low, moderate, high and very high) according to their thrombotic risk. The prevalence of VTE, deep vein thrombosis (DVT) and PE in each group was calculated. The odds of PE for pneumonectomy were also calculated and compared to lobectomy.
ResultsEleven patients (0.18%) had postoperative VTE. The mean age of this subset was 65.95 years; 90.9% were diagnosed with malignant neoplasm. Some 80.8% of patients in the series and all VTE cases were included in the high risk VTE group. VTE was more common in pneumonectomy (45.45% of VTE cases, odds ratio 4.6 compared to lobectomy).
ConclusionsThe prevalence of VTE in this series was 0.18% (1.31% in pneumonectomy patients). These figures could serve as reference values for thromboembolic disease in general thoracic surgery.
El objetivo de este estudio es determinar la prevalencia de la enfermedad tromboembólica venosa (ETV) en pacientes sometidos a intervenciones quirúrgicas torácicas programadas bajo un protocolo de profilaxis antitrombótica y determinar el riesgo de tromboembolismo pulmonar (TEP) en pacientes con resección pulmonar anatómica, comparando los casos de lobectomía y neumonectomía.
Pacientes y métodoEstudio descriptivo retrospectivo transversal en el que se incluyeron 6.004 pacientes sometidos a intervenciones quirúrgicas programada en nuestro centro y que recibieron profilaxis antitrombótica según protocolo. Los pacientes fueron distribuidos en grupos en función del riesgo trombótico en bajo, moderado, alto y muy alto. Se calculó la prevalencia de ETV, trombosis venosa profunda (TVP) y TEP en cada grupo y la odds ratio de TEP en los grupos de pacientes con neumonectomía y lobectomía.
ResultadosOnce pacientes presentaron ETV (0,18%). La edad media de estos pacientes fue de 65,95 años, el 90,9% tenían un diagnóstico de neoplasia y esta complicación fue más frecuente en neumonectomía (45,45% de los casos de ETV). El 80,8% de los pacientes presentaban un riesgo alto de ETV y el 100% de los casos de ETV se dio en pacientes de alto riesgo (0,23%). La odds ratio de ETV fue de 4.6 comparando los casos de neumonectomía y lobectomía.
ConclusionesLa prevalencia de ETV en esta serie, en la que se ha seguido una pauta estandarizada de profilaxis es de 0,18% (1.31% en pacientes neumonectomizados). Estas cifras pueden ser utilizadas como valores de referencia en Cirugía Torácica.
Deep vein thrombosis (DVT) and pulmonary embolism (PE), both clinical expressions of the same entity, venous thromboembolism (VTE), are major surgery-related complications.
The incidence of DVT exceeds 20% in patients undergoing major surgery, and may even reach 40% in cases of major orthopedic surgery.1 The risk of post-operative PE may reach 5% in patients with a high thrombotic risk, and is associated with 1%–10% of hospital deaths.2 It is the most common cause of preventable mortality in hospital.
Numerous studies have described the prevalence of VTE in patients undergoing major surgery. However, little is known to date about its prevalence in the thoracic surgery post-operative period, and few authors have studied this problem.3 The aim of this study was to define the prevalence (overall and by risk groups) of thromboembolic complications in patients undergoing elective thoracic surgery, to quantify the risk of PE in pneumonectomy compared to patients undergoing lobectomy, and to characterize the risk of suffering a VTE.
Patients and MethodsPatientsWe conducted a descriptive, cross-sectional study on a consecutive cohort of patients whose data were collected prospectively in a computer database. All patients operated on consecutively in our hospital and who underwent any elective thoracic surgery procedure with general anesthesia between December 1994 and April 2012 were included. Data quality control was assured by two successive audits of each hospital discharge report by a records manager (G.V.). The first was performed at the time of discharge and the second before sending the documentation to the hospital's medical record central archive, once all the information on the episode that was not available at the time of patient discharge had been included.
Patients received antithrombotic prophylaxis according to the SEPAR protocol in force at the time of surgery. The protocols included the recommendation for early ambulation, use of anti-coagulant drugs and mechanical measures among others. The drug used was low molecular weight heparin (LMWH). All patients in whom prophylaxis with anti-coagulant drugs was indicated were given a preoperative dose the day before surgery and the anticoagulation therapy was restarted during the immediate postoperative period. Patients underwent intense postoperative respiratory physiotherapy, which involved early ambulation. After discharge, LMWH was maintained for two weeks in patients who underwent major lung resection (lobectomy and pneumonectomy). The administration of LMWH on an outpatient basis was not recommended in the remaining patients. In patients with a very high thrombotic risk, prophylaxis with anticoagulant drugs was combined with mechanical measures (elastic compression stockings and intermittent compression stockings); this was the only measure used in patients with a very high bleeding risk.
Patients who underwent major lung resections were re-assessed in outpatients one month after surgery, while the remaining patients were followed-up by their respective referring doctors in their referral centers in accordance with their follow-up protocols; information concerning the patient was sent to our department in the case of complications.
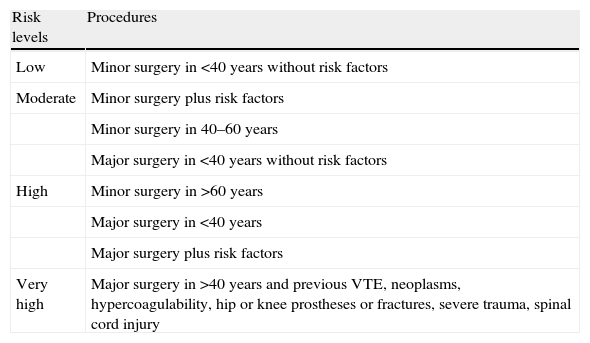
Following the SEPAR protocol in force at present,4 patients were distributed into groups depending on the thrombotic risk (low, moderate, high and very high) as described in Table 1.
Risk Levels for Venous Thromboembolism in Surgical Patients According to Guideline “Prophylaxis of Venous Thromboembolism” of the SEPAR Guidelines.5
| Risk levels | Procedures |
| Low | Minor surgery in <40 years without risk factors |
| Moderate | Minor surgery plus risk factors |
| Minor surgery in 40–60 years | |
| Major surgery in <40 years without risk factors | |
| High | Minor surgery in >60 years |
| Major surgery in <40 years | |
| Major surgery plus risk factors | |
| Very high | Major surgery in >40 years and previous VTE, neoplasms, hypercoagulability, hip or knee prostheses or fractures, severe trauma, spinal cord injury |
VTE, venous thromboembolism.
Minor surgeries were considered as those in which less complex, shorter (between 15 and 60min) surgical procedures were used, even though they were performed under general anesthesia.
Major surgeries were considered the more complex procedures, performed under general anesthesia and respiratory support, which entailed a certain degree of risk to the patient's life or serious disability.
The VTE diagnostic protocol was established when there was clinical suspicion of VTE and confirmation with additional diagnostic tests such as computed tomography angiography (angioCT) (in the case of PE) and echo-Doppler (in the case of DVT). In the case of sudden death of the patient, the diagnosis of VTE was established by multidisciplinary consensus in accordance with the clinical data.
VariablesThe variables analyzed, both demographic and pre- and intraoperative, were as follows: demographic (age, sex), body mass index (BMI), type of surgery (major/minor), diagnosis (neoplastic/non-neoplastic), presence or absence of risk factors for VTE, occurrence or not of VTE (DVT, PE or DVT+PE), thrombotic risk (very high, high, moderate and low) and mortality (hospital/post-discharge).
A descriptive analysis was performed on the demographic characteristics of the population, and thromboembolic episodes reported in the postoperative period were detailed. Patients were grouped according to the development of VTE during the postoperative period (VTE group and non-VTE group), and the demographic characteristics of both groups were compared. Likewise, patients were stratified according to the preoperative thrombotic risk (Table 1) into three risk subgroups (high/very high, moderate and low) for subsequent analysis and comparison of the frequency of thromboembolic episodes observed.
Statistical AnalysisThe variables were collected in a computer database for subsequent processing using the SPSS statistical package (SPSS Inc., Chicago, IL, USA), version 17.0 for Windows. The qualitative variables were expressed coded as number and percentage, and the quantitative variables as mean±standard deviation (SD), unless the distribution was not normal, in which case they were expressed as median and range. The quantitative variables were compared using the Student's t-test for independent samples. If the distribution was different from normal, or the sample size was small, a non-parametric test was used (Mann–Whitney U-test). The difference between variables was considered statistically significant when the P-value was less than or equal to 0.05. Quantification of the risk of PE in the patient populations with lobectomy or pneumonectomy was carried out in 2×2 tables by calculating the odds ratio and its 95% confidence interval.
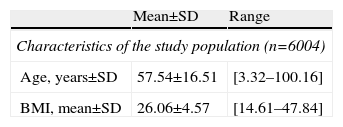
ResultsBetween January 1994 and November 2011, 6004 patients underwent elective thoracic surgical procedures under general anesthesia. The demographic and preoperative data for the study group are documented in Table 2. Lobectomy was performed in 1378 cases and pneumonectomy in 305 patients. Among the remaining surgeries, 118 bilobectomies, 59 typical and 1238 atypical segmentectomies, 289 lung biopsies, 137 chest wall resections, 74 thymectomies and 168 thyroidectomies were performed, among others. Among the diagnoses, lung cancer was the most common (2245 cases); 522 cases of lung metastases, 442 cases of spontaneous pneumothorax, 321 cases of pulmonary nodule, 211 cases of pleural effusion, 178 cases of interstitial lung disease, 161 cases of goiter, 149 cases of tracheal stenosis, 115 cases of sarcoidosis, 108 cases of chest wall tumors and 92 cases of thymomas were recorded, among others. The most common risk factors presented by patients in our series were age over 60 years (54%), obesity (18.1%) and history of cancer (68.7%).
Demographic Characteristic and Preoperative Data.
| Mean±SD | Range | |
| Characteristics of the study population (n=6004) | ||
| Age, years±SD | 57.54±16.51 | [3.32–100.16] |
| BMI, mean±SD | 26.06±4.57 | [14.61–47.84] |
| n | % | |
| Sex, males | 4451 | 74.1 |
| Presence of risk factors | 3877 | 64.6 |
| Diagnosis of neoplasm | 3723 | 62 |
| Major surgery | 4530 | 75.4 |
SD, standard deviation; BMI, body mass index.
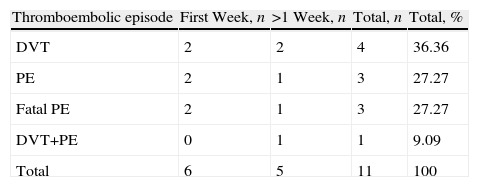
Eleven patients had some thromboembolic episode, representing a prevalence of 0.18% in the study group. Of these, six cases presented in the form of PE, four as DVT and one as PE concomitant with DVT. Some 54.5% of the thromboembolic episodes occurred within the first week postoperatively, as detailed in Table 3, and in four cases the diagnosis was made after discharge.
None of the cases of DVT died as a result of the thrombotic episode and all progressed well after the diagnosis and treatment of the complication. Among the seven cases with PE, three deaths were recorded (42.86%), one post-discharge, representing a mortality due to PE in the overall series of 0.05%.
The primary diagnosis among patients who developed PE was lung cancer (6 cases: 2 squamous cell carcinoma, 2 adenocarcinoma, 1 bronchioloalveolar and 1 large cell) and colon cancer lung metastases (one case). Among the patients who developed DVT, the primary diagnosis was lung cancer (3 cases: 2 squamous cell carcinoma and the other adenosquamous) and benign pulmonary nodule (one case).
The seven patients who presented PE had undergone major surgical procedures, which included: 4 pneumonectomies (3 right and 1 left), 2 lobectomies and 1 atypical segmentectomy. The three patients who underwent right pneumonectomy and who presented PE in the postoperative period died, during the first, seventh and fifteenth day postoperatively, respectively. The four patients who presented DVT had undergone one atypical segmentectomy, one extended left pneumonectomy, one lower middle bilobectomy and one lobectomy with bronchoplasty.
Only one patient who presented DVT as a complication following an extended left pneumonectomy had received chemotherapy prior to the surgery.
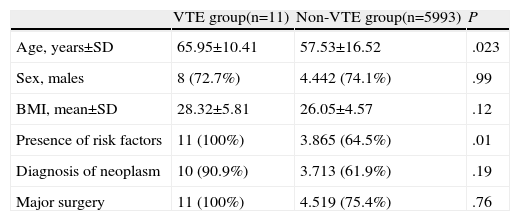
Stratification Into Subgroups: ResultsPatients who presented thromboembolic complications (VTE group) had two or more risk factors, such as advanced age, obesity, surgery due to cancer, history of DVT or presence of varicose veins, among others. The results of the comparative analysis between groups (VTE vs non-VTE) are shown in Table 4. Patients in the VTE group had a higher mean age (65.95±10.41 vs 57.53±16.52, P<.05) and body mass than patients in the non-VTE group, as well as a diagnosis of neoplasm in more than 90%; all had undergone major thoracic surgery.
Comparison of General Conditions Between Groups.
| VTE group(n=11) | Non-VTE group(n=5993) | P | |
| Age, years±SD | 65.95±10.41 | 57.53±16.52 | .023 |
| Sex, males | 8 (72.7%) | 4.442 (74.1%) | .99 |
| BMI, mean±SD | 28.32±5.81 | 26.05±4.57 | .12 |
| Presence of risk factors | 11 (100%) | 3.865 (64.5%) | .01 |
| Diagnosis of neoplasm | 10 (90.9%) | 3.713 (61.9%) | .19 |
| Major surgery | 11 (100%) | 4.519 (75.4%) | .76 |
SD, standard deviation; VTE, venous thromboembolism; BMI, body mass index.
When patients were stratified into groups according to the preoperative thrombotic risk factor (high/very high, moderate and low), the comparative analysis showed a statistically higher prevalence of VTE in patients with a high thrombotic risk (0.23% vs 0%). None of the patients belonging to the moderate and low risk groups had thromboembolic episodes.
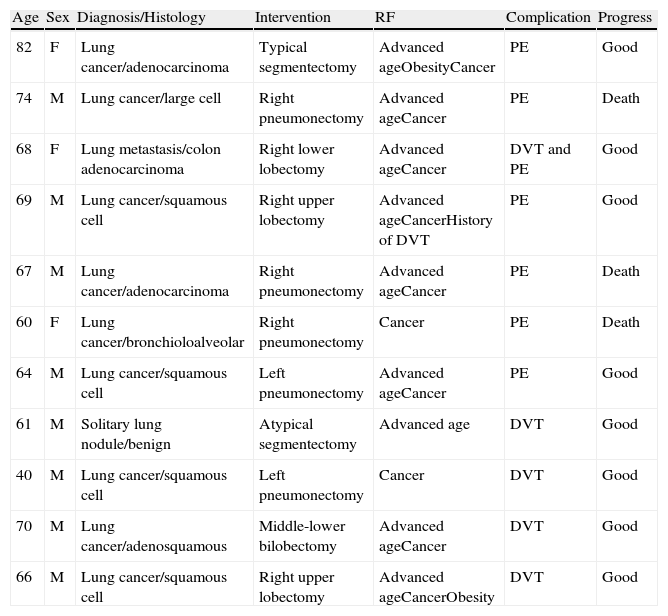
Table 5 shows the characteristics of the 11 patients who had thromboembolic complications.
List of the 11 Patients Who Presented Venous Thromboembolism.
| Age | Sex | Diagnosis/Histology | Intervention | RF | Complication | Progress |
| 82 | F | Lung cancer/adenocarcinoma | Typical segmentectomy | Advanced ageObesityCancer | PE | Good |
| 74 | M | Lung cancer/large cell | Right pneumonectomy | Advanced ageCancer | PE | Death |
| 68 | F | Lung metastasis/colon adenocarcinoma | Right lower lobectomy | Advanced ageCancer | DVT and PE | Good |
| 69 | M | Lung cancer/squamous cell | Right upper lobectomy | Advanced ageCancerHistory of DVT | PE | Good |
| 67 | M | Lung cancer/adenocarcinoma | Right pneumonectomy | Advanced ageCancer | PE | Death |
| 60 | F | Lung cancer/bronchioloalveolar | Right pneumonectomy | Cancer | PE | Death |
| 64 | M | Lung cancer/squamous cell | Left pneumonectomy | Advanced ageCancer | PE | Good |
| 61 | M | Solitary lung nodule/benign | Atypical segmentectomy | Advanced age | DVT | Good |
| 40 | M | Lung cancer/squamous cell | Left pneumonectomy | Cancer | DVT | Good |
| 70 | M | Lung cancer/adenosquamous | Middle-lower bilobectomy | Advanced ageCancer | DVT | Good |
| 66 | M | Lung cancer/squamous cell | Right upper lobectomy | Advanced ageCancerObesity | DVT | Good |
RF, risk factor; F, female; M, male; PE, pulmonary embolism; DVT, deep vein thrombosis; CT, computed tomography.
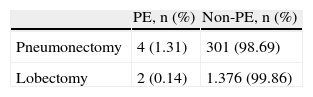
In the lobectomy cases, the prevalence was 0.15 (3/1.378) and in the pneumonectomy, 1.31 (4/305; odds ratio: 9.14 95% CI, 1.30–101.29) (Table 6).
DiscussionAll surgical procedures generate a state of venous stasis and hypercoagulability, as well as a certain level of endothelial damage, the three factors that bring together Virchow's triad and which favor the development of VTE in these patients. VTE is a major complication that affects hospitalized patients and which is closely related with surgery.
Various studies have described its prevalence in patients undergoing specific chest procedures. Thus, in a study by Ziomek et al.5 in which 77 patients who underwent lung resection surgery for lung cancer were analyzed, 20 patients (26%) had a thromboembolic episode in the postoperative period; there were 15 cases of DVT and 5 cases of PE. According to other authors, the mortality derived from these thromboembolic complications varies between 15% and 20%.6 Kalweit et al.7 analyzed 1735 patients who underwent lung resection surgery. In their series, PE was the second most common cause of death during the postoperative period, accounting for 15.2% of deaths post-resection. The high incidence of thromboembolic complications observed in these series could be due to a lack of standard protocols for heparin thromboprophylaxis, as happened previously in the 1990s. In a more recent study, Dentali et al.8 described, in a series of 693 patients who underwent thoracotomy for lung cancer under an antithrombotic prophylaxis protocol, an incidence of VTE and PE of 1.7% and 1.3%, respectively, with 0.6% mortality attributed to PE. These figures are more similar to those obtained in our series, in which eight patients of the 1749 who underwent lung resection surgery for lung cancer had thromboembolic complications (0.005%), with a mortality due to this cause of 0.002%.
The incidence of VTE in surgical patients without prophylaxis may reach 80% in patients with a very high thrombotic risk.4 However, although most patients undergoing elective thoracic surgery procedures have a high or very high thrombotic risk due to their characteristics (80.8%), in our study the prevalence of VTE was 0.18%. This low prevalence may be attributable to the use of thromboprophylaxis protocols, which include the use of anticoagulant drugs and mechanical measures (intermittent compression systems and elastic stockings) and early ambulation, following international recommendation guidelines.9 Taking these data into account, it is vitally important to perform an individualized assessment of each patient, determining their thrombotic risk in order to apply the best thromboprophylaxis possible based on the latest recommendations in the guidelines.
The postoperative period in thoracic surgery represents an increased risk of VTE, both due to the advanced age of the patients and the high frequency of neoplastic diseases as a reason for the intervention. Although the precise prevalence of VTE is unknown, we do know that the incidence of DVT in people aged 65–69 years is 1.8 cases/1000 persons/year and increases to 3.1 cases/1000 persons/year between 85 and 89 years.10 In our series, the mean age of the patients who presented VTE was 65.95 years, considerably older than the group of patients who did not have this complication (57.53 years).
The presence of neoplasm increased the risk of VTE between six- and sevenfold, and the development of PE threefold.11,12 According to a recent systematic review in which 26 studies were assessed, the prevalence of PE in patients with lung cancer was 3.6%.13 In our series, 90.9% of patients who had VTE were diagnosed with neoplasm, either primary or metastatic, which was the reason for the surgery.
Among patients who undergo surgical resection due to oncological processes, VTE is considered a major cause of mortality and may serve as an important predictor of survival. According to De Martino et al.,14 the variation in the risk of VTE among patients undergoing surgical resection not only depends on the type of cancer, but is also associated with the magnitude of the surgery necessary for the resection. In the case of surgery due to lung cancer, they reported an incidence postoperatively or within the first 30 days after surgery of DVT, PE and VTE of 1.3%, 1.3%, and 2.3%, respectively. Interestingly, the hospital stay (>1 week) is established as one of the major risk factors associated with VTE. Lyman et al.15 established that the risk of having a fatal PE after surgery for lung cancer is three times higher than in patients undergoing the same surgery for benign causes.
Pneumonectomy is associated with a higher rate of complications and mortality than any other thoracic surgery procedure. Patients undergoing pneumonectomy have a higher risk of VTE than patients undergoing lobectomy for stage I and II lung cancer, due to greater activation of coagulation, which appears from the seventh postoperative day.16 These data are consistent with those observed in our series, where patients who had VTE had undergone pneumonectomy (5 cases), the most common surgical procedure, three of whom died during the postoperative period as a result of a PE (all had undergone right pneumonectomy). There are several studies that have determined the prevalence and mortality associated with thromboembolic episodes in patients undergoing pneumonectomy due to lung cancer. Mason et al.17 analyzed 336 patients, of whom 25 presented a thromboembolic episode after the pneumonectomy (17 cases of DVT, 5 cases of PE and 3 cases of DVT+PE), with a maximum peak incidence on the seventh day postoperatively. With respect to mortality, Weder et al.,18 in their series of 176 patients who underwent pneumonectomy due to lung cancer after neoadjuvant chemotherapy, described a mortality of 3%; half were attributed to pulmonary thromboembolic complications. However, in our series, the prevalence of thromboembolic complications in patients who underwent pneumonectomy was lower than that described by other authors: 0.32% for DVT and 1.3% for PE. This low prevalence may be explained by the use of anti-thrombotic prophylactic protocols with anticoagulant drugs, and by the use of mechanical measures employed comprehensively and routinely in our hospital.
Seven of the patients who presented VTE in our series developed the complication while in hospital. Therefore, it is important to carry out close clinical follow-up with a high level of suspicion for early diagnosis of these complications. In four of the cases with VTE, the complication appeared after discharge. Thus, in patients with a high thrombotic risk, such as neoplastic patients in whom oncological surgery is performed, prophylaxis is recommended for 2–3 weeks after discharge.4 According to the results of two randomized studies, prolonging the duration of anticoagulation treatment beyond four weeks after surgery reduces the risk of VTE.19,20
There are more than 20 international guidelines that recommend VTE prophylaxis in high risk patients. The recent Antithrombotic Therapy and Prevention of Thrombosis guidelines from the American College of Chest Physicians (9th edition), recommends the use of LMWH, unfractionated heparin (UFH) or intermittent pneumatic pressure stockings in patients with moderate thrombotic risk. For patients with high thrombotic risk and low bleeding risk, it recommends the use of LMWH, UFH and mechanical measures, with either elastic stockings or intermittent pneumatic pressure stockings. In patients with a high bleeding risk, the use of mechanical measures is recommended, preferably intermittent compression systems, until the risk of bleeding decreases and pharmacological prophylaxis can be started. In our series of patients who underwent elective thoracic surgery, routine follow-up of these anti-thrombotic prophylactic protocols based on a thrombotic risk stratification has been shown to be highly efficient, with a low prevalence of VTE (0.18%) and excellent results.
This study has some significant limitations. Firstly, all the techniques for establishing the diagnosis of VTE were not used in all patients with radiological changes and postoperative dyspnea, so the real prevalence of VTE may be different to that described in our results. Furthermore, this is a retrospective study, so it is impossible to establish causality between the different thoracic surgery procedures and thromboembolic complications. Although data collection was prospective, there could be bias in the collection of risk factors in cases that presented the complication compared to those that did not. An active search for thromboembolic complications was carried out in all patients in the series, although autopsies were not performed on all patients, so PE could be the unsuspected cause of death in any patient who had another type of complication. Nevertheless, the results obtained in our series could be used to conduct prospective cohort studies designed to validate the risk of VTE in patients undergoing thoracic surgery procedures.
ConclusionsPatients undergoing elective thoracic surgery have a low prevalence of VTE (0.18%), attributable to the use of anti-thrombotic prophylaxis protocols based on proper stratification of thrombotic risk. However, in patients undergoing lung resection, especially in pneumonectomies, the risk is not inconsiderable and this complication should be taken into account as a priority suspected diagnosis in patients with acute respiratory episodes. The figures may be used as reference values, as they have been extracted from a large series with prospective records and uniform diagnostic criteria.
FundingThe authors declare that they have not had any funding to conduct this study.
Conflict of InterestsThe authors declare that there are no conflicts of interests of any type in relation to the publication of this document.
Please cite this article as: Gómez-Hernández MT, et al. Prevalencia de la enfermedad tromboembólica venosa en cirugía torácica programada. Arch Bronconeumol. 2013;49:297–302.