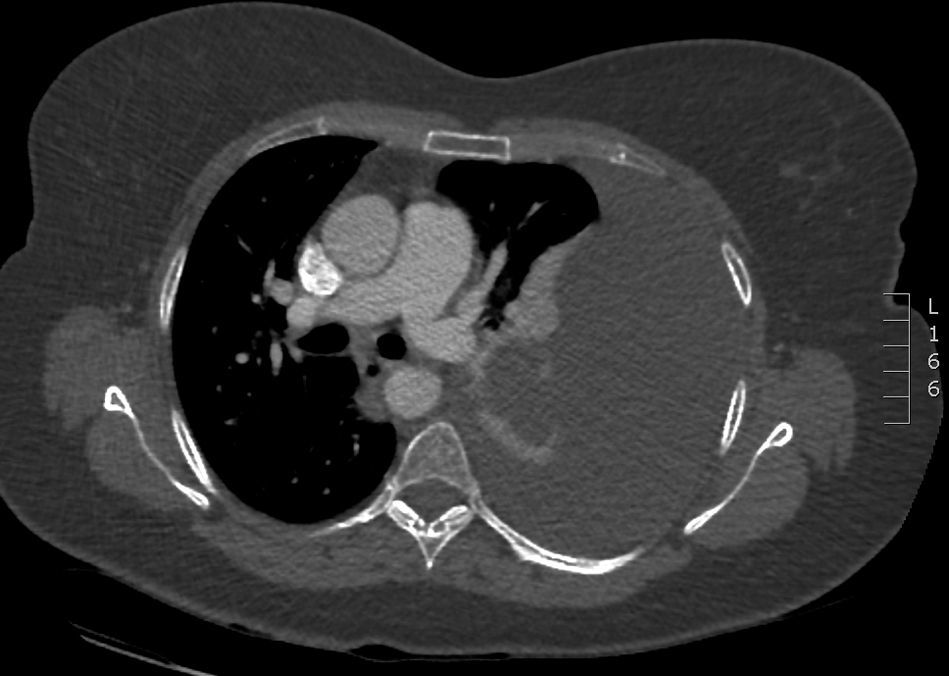
We report the case of a 49-year-old woman, non-smoker, with arterial hypertension and asthma, who presented in our hospital with an approximately 2-week history of dyspnea and chest pain. She was diagnosed with left pleural effusion (Fig. 1). We performed thoracocentesis to evacuate fluid for symptomatic relief. The fluid obtained was opalescent, consistent with sparsely cellular exudate, with normal adenosine deanimase (ADA) values, and negative cytology and microbiology. The usual causes of exudate were ruled out by imaging studies (echocardiogram, computed axial tomography) and clinical laboratory tests (complete blood count, kidney and liver function, and autoantibodies [ANAS, ANCAS and lupus anticoagulant] negative) and no diagnosis was reached. Single port video-assisted thoracoscopy (VATS) was then performed, showing, after evacuation of the effusion, a pleural tumor measuring 5×5cm in the posterior sulcus. An anterolateral thoractomy was necessary to resect the lesion from the pleura with 2cm margins of healthy pleura around the pedicle, after confirming that it did not infiltrate any other structure. Immunohistochemical studies were performed, showing positivity for CD31 and factor 8, and a Ki67 proliferation index <5%, yielding a definitive diagnosis on pathology of pleural capillary hemangioma.
Hemangiomas are neoplasms characterized by vascular proliferation, and are sometimes confounded with other diseases such as arteriovenous vascular malformations.1 They are classified as cavernous or capillary, depending on the diameter of the vascular channels comprising the tumor.2
The pathogenesis of hemangiomas is unknown. They can be found in any part of the body, although they most typically appear on the skin and in the liver, and are very rarely found in sites such as the chest. It is even more rare to find them in the ribs3 or the mediastinum, where they occur at incidence of 0.5% of all masses in these sites.4 To our knowledge, only 2 cases of pleural hemangioma have been described to date. One of these was accompanied by bloody pleural effusion,1 as might be expected, and the other presented with non-bloody effusion, but was cavernous5 rather than capillary as in our case. Most hemangiomas are observed in young adults, before the age of 35 years. They are usually found by chance or after spontaneous rupture causing bleeding or hemorrhagic pleural effusion. Symptoms are generally non-specific, and include cough, chest pain and dyspnea,1 as seen in our patient. Treatment must be individualized, depending on the site and depth of the infiltration.5 The most usual approaches are surgical resection (as in our patient), cryotherapy, embolization or vascular ligation. Corticosteroids and cyclophosphamide have also been used. It is unusual for hemangiomas to relapse, and our patient is no exception: she has not had any recurrence of pleural effusion in the 5 months since surgery.
In conclusion, this is a case of capillary hemangioma located in the pleura, an extremely rare location, accompanied by non-hemorrhagic pleural effusion, an unexpected presentation in this type of tumor.
Our thanks to Dr Luis Molinos Martín for his help in writing this report.
Please cite this article as: Yoldi LAS, Vigil LV, Solis RA. Derrame pleural secundario a un hemangioma capilar de localización pleural. Arch Bronconeumol. 2016;52:537.