Nuclear carcinoma of the testis (NUT) is very rare tumors with specific genetic changes that progress very aggressively. They often affect children and young adults. They may occur in different organs, but they are characteristically located in the midline of the head and neck.1 Very few cases have been published that describe this entity in the lungs and mediastinum.
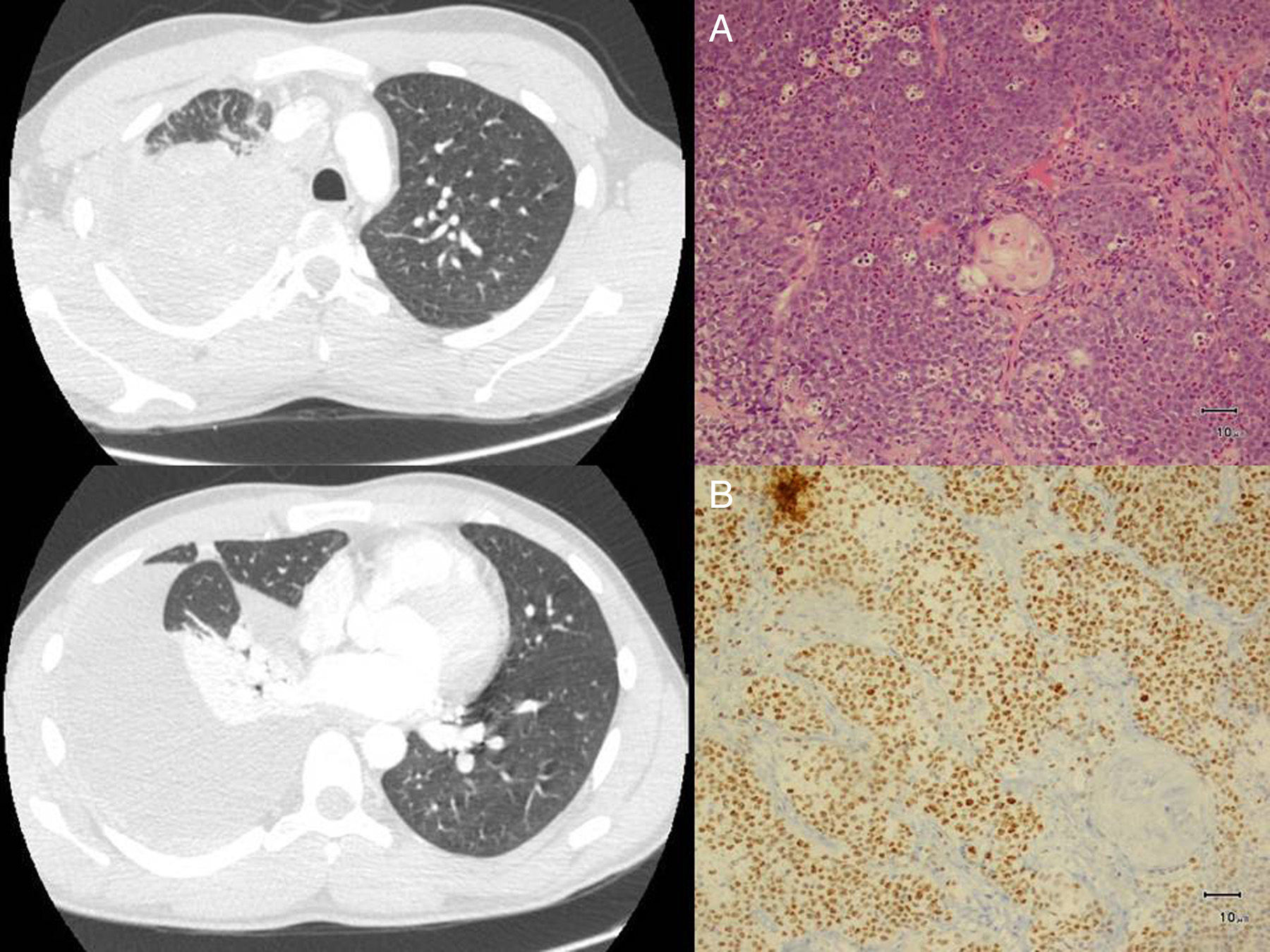
We report the case of a 23-year-old man, smoker of about 10 cigarettes/day, who presented in our hospital with a 2-week history of pain in the right hemithorax radiating to the shoulder, and asthenia. Computed tomography (CT) showed increased density without air bronchogram occupying the posterior and apical segments of the right upper lobe (RUL) with amputation of the corresponding segmentary bronchi, paratracheal mediastinal lymphadenopathies, and significant right pleural effusion (Fig. 1). Given these findings, a positron emission tomography (PET) was performed, revealing a metabolically positive mass in the RUL, with extensive pleural involvement in the same side, mediastinal lymph node involvement, and bilateral supra/infraclavicular lytic bone lesions and metastasis. Fiberoptic bronchoscopy revealed complete stenosis of the posterior and apical segments of the RUL bronchus due to thickened, hypervascularized mucosa, possibly of a neoformative origin. Diagnostic confirmation was obtained from a pleural biopsy obtained by thoracoscopy. The pathology report described a neoplasm formed of nests of undifferentiated cells, and, along with this cell population, abrupt areas of squamous differentiation. The undifferentiated tumor cells showed positive immunoreaction to NUT antibody and pancytokeratin (Fig. 1).
Given the definitive diagnosis of NUT carcinoma, the patient received 2 cycles of palliative chemotherapy with cisplatin and etoposide, and then stared BET inhibitor therapy in a clinical trial setting. The oncological disease did not respond to treatment, and the pulmonary mass increased in size, with compression of the superior vena cava and pericardial effusion. The patient died 3 months after the initial diagnosis.
NUT carcinomas are poorly differentiated and genetically defined by the presence of a genetic rearrangement of the NUT gene, consisting of a chromosomal translocation between this gene (NUTM1) located in the chromosome 15q14 and other genes (BRD4 in chromosome 19p13.1 [70%], BRD3 in chromosome 9q34.2 [6%] or an unknown gene [24%]).2 The incidence is unknown, but this tumor is considered rare. It was originally thought to be a disease of children and young adults, but subsequent publications have shown that NUT carcinoma can equally affect individuals of any age and both sexes.
The tumor generally occurs in the midline structures, usually associated with the upper gastrointestinal tract, but it has been identified in other sites. According to reports in the literature, only 38 cases of primary intrathoracic NUT are known, of which 19 were of pulmonary origin.3
In histopathological terms, it is very similar to squamous carcinoma, and therefore may be underdiagnosed. If NUT is suspected, diagnostic confirmation is obtained with immunohistochemical techniques, as in our patient, or by the detection of chromosomal rearrangement of the specific NUT variants.3
To date, no specific treatment exists for NUT carcinoma. The rapid growth and aggressivity of this tumor rules out surgical treatment, and it does not appear to respond to most chemotherapeutic regimens and/or radiation therapy, although the best option appears to be a combination of gemcitabine, docetaxel and cisplatin. Some promising therapies, such as vorinostat and BET inhibitors, are currently under study and perhaps these will provide an effective treatment in the future.4 However, the current prognosis for this entity is death after a mean period of survival of around 7 months,5 as occurred in our case. To conclude, NUT carcinoma is extremely rare and very aggressive, so early clinical suspicion of this entity of utmost importance to avoid delays in establishing the most specific treatment possible in the shortest time.
Please cite this article as: Benito Bernáldez C, Romero Muñoz C, Almadana Pacheco V. Carcinoma NUT pulmonar, una forma poco frecuente de cáncer de pulmón. Arch Bronconeumol. 2016;52:619–621.