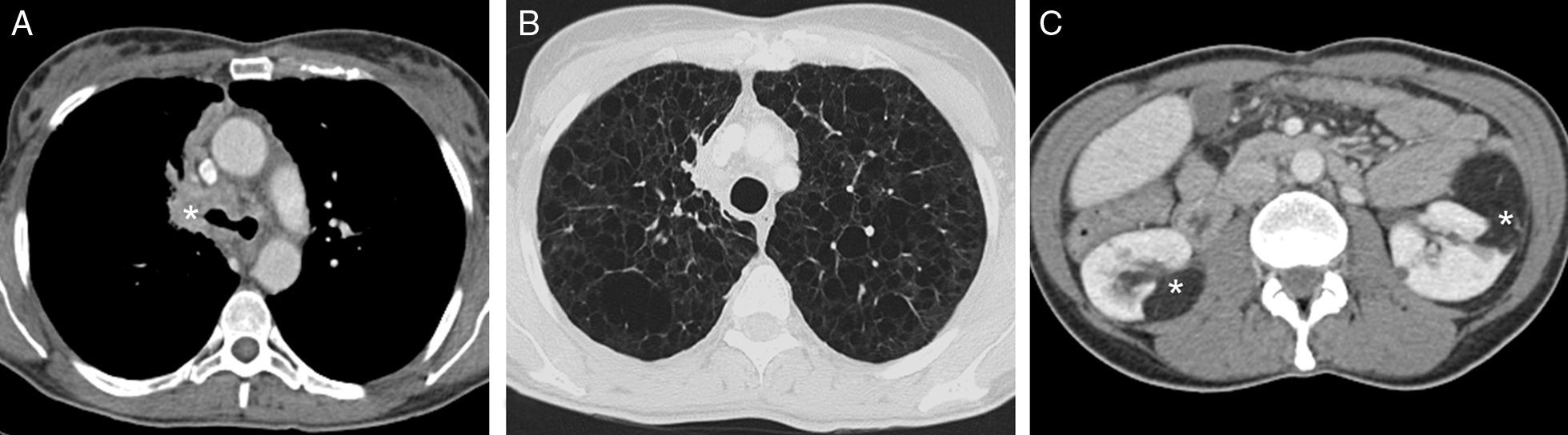
We report the very rare case of a 47-year-old woman, former smoker (with an accumulated pack-year index of 10), who consulted due to hemoptysis. The most notable aspect of her clinical history was a sporadic form of lymphangioleiomyomatosis (LLM) diagnosed in her childhood as a result of a bleeding renal angiomyolipoma. A chest radiograph showed paramediastinal opacity in the right upper lobe. A chest computed tomography (CT) confirmed a tumor involving the right primary bronchus, infiltrating the tracheal carina and the mediastinum (Fig. 1A), and multiple pulmonary cysts with thin, well-defined walls (Fig. 1B). Multiple renal angiomyolipomas (AML) were seen in the upper abdomen (Fig. 1C). Adenocarcinoma was confirmed by bronchial biopsy. The patient is receiving chemotherapy, with partial response to treatment.
(A) Axial image of chest CT (mediastinal window), showing a central mass involving the right primary bronchus and the tracheal carina (asterisk). (B) Axial image of chest CT (pulmonary parenchymal window), showing multiple thin-walled cystic lesions distributed diffusely throughout both lungs. (C) Axial CT image of the abdomen, showing multiple bilateral solid renal tumors with fat attenuation (asterisks) consistent with angiomyolipomas.
LLM is a rare systemic disease, described almost exclusively in women of childbearing age, characterized by interstitial proliferation of smooth muscle that particularly affects the lung. The usual radiological finding in this disease is the presence of multiple cystic lesions distributed diffusely throughout both lungs. Pulmonary neoplasms associated with LLM include some isolated cases of pulmonary AML, multifocal micronodular pneumocyte hyperplasia, and clear cell (sugar) tumor, but only 2 cases of lung cancer have been published in the scientific literature.1,2
Please cite this article as: Gorospe Sarasúa L, Mercedes-Noboa E, Olmedo-García ME. Carcinoma broncogénico en paciente con linfangioleiomiomatosis. Arch Bronconeumol. 2017;53:342.