Valve lung volume reduction (LVR) is being increasingly used for selected patients with severe emphysema. It is associated with a good safety and efficacy profile; however, even patients considered suitable candidates may develop severe complications and may not respond to treatment.
We present the case of a 60 year-old female patient, suffering from stage IV chronic obstructive pulmonary disease (COPD) associated with severe dyspnoea on exertion and non-hypercapnic respiratory failure. Pulmonary function tests (PFTs) showed severe airflow obstruction (FEV1 0.57 L, 24% predicted), and hyperinflation (RV 334% predicted, FRC 274% predicted). Radiological assessment revealed advanced bilateral heterogeneous emphysema, with upper lobe predominance. Medical treatment optimization and pulmonary rehabilitation did not result in clinical improvement.
Lung volume reduction (LVR) surgery was rejected by the patient due to its non-reversibility, so she was evaluated for endoscopic LVR. A ventilation/perfusion scan confirmed high ventilation/perfusion heterogeneity with bilateral upper-lobe hypo-perfusion. The low tissue density was considered a relative contraindication for the implantation of endobronchial coils.1 Based on these findings, the patient was considered a suitable candidate for bronchoscopic LVR using endobronchial valves.2
Target lobe selection was made with the ChartisTM system,3 which revealed significant collateral ventilation in all lobes, except in the right upper lobe (RUL). Three valves (Zephyr®, Pulmonx Inc., Redwood City, CA, USA) were inserted in the 3 segmental bronchi of the RUL. The procedure achieved RUL atelectasis, but was immediately complicated by right tension pneumothorax, which was treated by chest tube insertion. Due to a persistent air-leak, and following current recommendations,4 the endobronchial valve situated in the anterior segmental bronchus was removed 15 days after the initial procedure to halt the active air-leak and remove the chest drain.
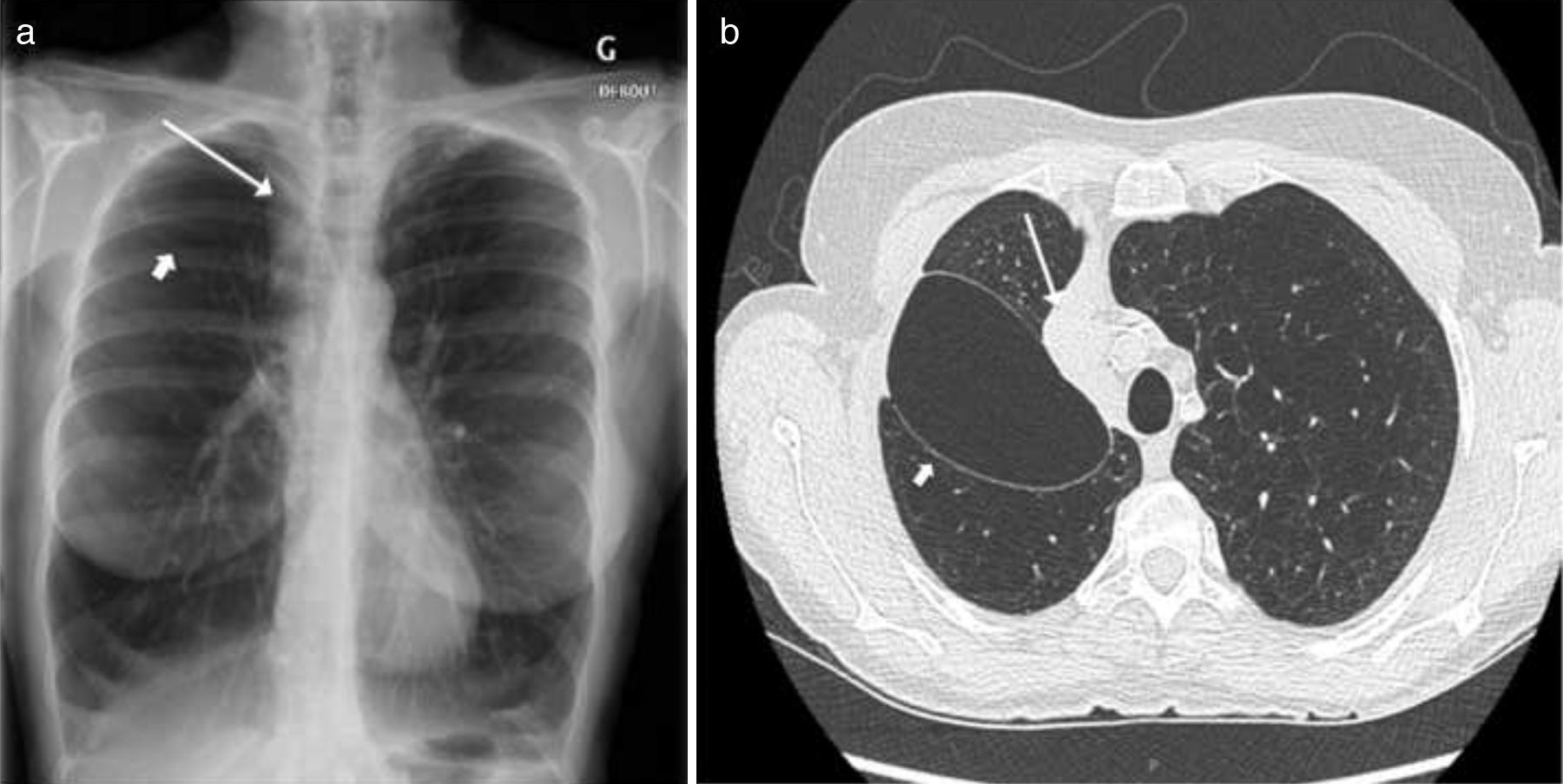
During the following 3 months, no significant clinical or functional improvement was observed. The imaging studies revealed an unresolved interlobar air cavity and persistent RUL atelectasis (Fig. 1). It was suspected that this voluminous cavity counterbalanced the benefit of volume reduction obtained by RUL atelectasis, and thus, the remaining valves were removed. The apical valve was inaccessible due to bronchial angulation; however, the posterior one was removed successfully.
Despite removal of the second valve, RUL atelectasis and interlobar air cavity persisted. A chest tube was then placed inside the air cavity under CT guidance, and revealed a perpetual air-leak, explaining the long-lasting pneumothorax (for more than 3 months, after the initial procedure). The patient was referred for thoracic surgery to restrain the pneumothorax and to achieve lung reduction. Due to lobar atelectasis, a right upper lobectomy was chosen instead of a classical LVR surgery. This procedure halted the air leak, permitting removal of the chest drain after 3 days. At clinical follow-up, several months after the surgical LVR, no significant clinical or functional improvement was observed and the patient was referred for lung transplantation evaluation.
In our case, multiple complications developed, including a “classical” procedure-related pneumothorax associated with valve-induced atelectasis and a very long-standing air-leak associated with a residual air-cavity.
Pneumothorax is common after valve LVR, arising in approximately 10% of cases.4,5 It is usually the result of pleural or parenchymal tears following valve-induced atelectasis. However, this occasionally life-threatening complication is at the same time the pledge of clinical improvement. The absence of benefit in our patient, despite the persistent atelectasis, was initially attributed to the pneumothorax.
Prolonged air-leaks are known complications of valve LVR.4 However, to our knowledge, long-lasting pneumothorax, related to valve LVR, has not previously been described. In our case, 3 months after the initial valve implantation, a persistent interlobar air cavity was diagnosed. The differential diagnosis included an ex-vacuo pneumothorax or a low flow parenchymal-pleural fistula. Thoracic drainage confirmed a perpetual air leak proving the presence of a fistula. Subsequent failure to treat this air-leak with chest tube insertion motivated a surgical LVR.
This case shows how developing complications may outweigh the expected benefits of endoscopic LVR. Thoracic surgery may correct a complication related to the endoscopic procedure, reflecting the need for a multidisciplinary approach to investigate and treat these emphysema patients. Finally, current criteria for selection of endoscopic or surgical LVR candidates may have limitations in identifying “responders”. Large randomized studies could improve patient selection criteria.
Please cite this article as: Mitropoulou G, Casutt A, Lovis A. Fuga de aire prolongada, tras una reducción de volumen pulmonar con válvula que requirió lobectomía. Arch Bronconeumol. 2016;52:495–497.