Recent years have seen an increase in developed countries in the incidence of infections caused by environmental mycobacteria, particularly Mycobacterium avium complex (MAC) infection in immunocompetent patients; the primary radiological signs of this entity are fibrocavitary disease or nodules and bronchiectasis, predominantly in the middle lobe and lingula.1 This manifestation, known as Lady Windermere syndrome (LWS), has been described mostly in women over 50 years of age, while episodes in men are anecdotal.2
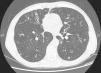
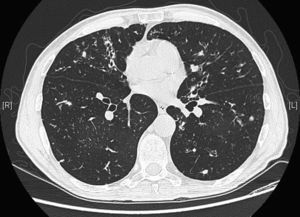
We report the case of a 64-year-old man, health worker, with no significant personal history or known toxic habits, who reported a 3-year history of non-productive cough, with no particular diurnal pattern, dysphonia and excess mucosity in the oropharyneal cavity, and additionally, in the last year, asthenia and recurrent episodes of low-grade fever. Forced spirometry results were as follows: FEV1/FVC 0.46; FEV1 1.91L (60%); FVC 4.14L (101%). Bronchodilator challenge and skin prick tests with allergens were negative. Computed tomography of paranasal sinuses, sweat chloride test, IgG, IgM, IgA, IgE and alpha-1 antitrypsin levels were all within normal ranges. A human immunodeficiency virus test was negative. A barium swallow study of gastroesophageal transit revealed gastric reflux. Chest CT showed bronchiectasis in the middle lobe and lingula associated with mucus plugs and distal centrilobular nodes (Fig. 1). Macroscopic results from fiberoptic bronchoscopy sampling were normal, while M. avium complex was isolated from bronchoalveolar lavage. The patient met diagnostic criteria for environmental mycobacteria published by the American Thoracic Society (2007)3 and was diagnosed as having MAC infection consistent with LWS.
In immunocompetent patients, MAC infection can present in 2 ways: (1) fibrocavitary lesions in the upper lobes, often observed in middle-aged men and often associated with a history of smoking and/or alcohol abuse and previous lung disease and (2) nodular lesions less than 5mm in size generally associated with bronchiectasis. These lesions occur predominantly in the middle lobe and lingula and are more common in women. This entity is known as LWS.4 This syndrome was first described in 1992 by Reich and Johnson in a series of 6 older, immunocompetent women with no significant history of smoking or previous respiratory disease who developed MAC infection. They postulated that voluntary suppression of the cough reflex predisposed to the syndrome by preventing secretion drainage. Moreover, other factors, such as leptin or adiponectin levels and menopause5 might also play a role in the pathogenesis of this infection. Our patient had chronic cough associated with gastroesophageal reflux, which he tried to suppress during his work that involved contact with the public, and this may have promoted the development of MAC infection. Despite the patient being a man, the clinical, microbiological and radiological criteria led to a diagnosis of LWS.
Please cite this article as: Gonçalves JMF, González JR. Síndrome de Lady Windermere. ¿Una entidad exclusiva de mujeres? Arch Bronconeumol. 2016;52:538–539.