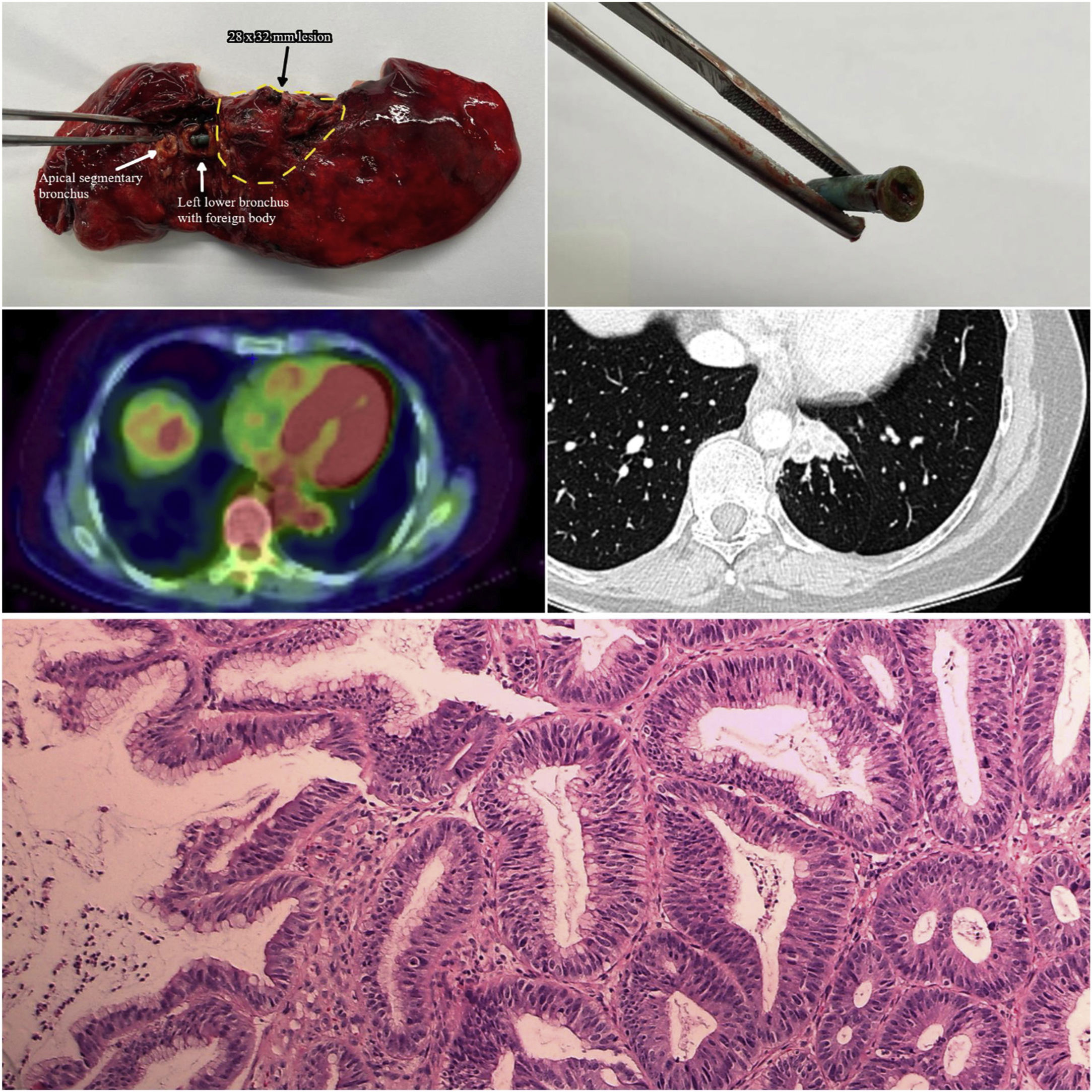
52 years-old woman presented persistent cough and single-episode haemoptysis, no clinical history. CT-scan showed hypoplastic left lower lobe with 28mm×32mm PET positive (SUVmax=2.7) lesion obstructing bronchus. Bronchoscopy showed non-transitable bronchial obstruction and oedema of mucosa. Biopsies suggested well-differentiated neoplasm (adenoma/adenocarcinoma G1). Mutational panel showed presence of BRAF mutation. Bronchial-sleeve left lower lobectomy was programmed. Frozen-section bronchial margin resulted negative and a 2.5cm plastic screw was found in the basal pyramid. Histology showed a pattern of giant-cell chronic inflammation without neoplasm. No mutations of BRAF were found in the specimen. Patient didn’t recall foreign-body inhalation during youth. Inveterate foreign-body inhalation is a rare problem in adults and left lower bronchus localization relatively uncommon (14% of cases).1 In this case foreign-body caused chronic inflammation and consequent tissue reaction mimicking a malignant process. Furthermore, bronchial obstruction prevented normal lobar development causing hypoplasia. The absence of radiological findings suggesting foreign-body (non-metal screw) addressed an endobronchial lesion (NSCLC/carcinoid/hamartoma) and the endoscopic biopsy with BRAF mutation constituted a challenging element for correct preoperatory diagnosis. However surgical approach was also prompted by the hypoplastic lobe, towards preventing potential uncontrollable haemoptysis or recurrent pneumonia and would have been the correct approach even with a correct preoperatory diagnosis (Fig. 1).
The Impact Factor measures the average number of citations received in a particular year by papers published in the journal during the two preceding years.
© Clarivate Analytics, Journal Citation Reports 2025
SRJ is a prestige metric based on the idea that not all citations are the same. SJR uses a similar algorithm as the Google page rank; it provides a quantitative and qualitative measure of the journal's impact.
See moreSNIP measures contextual citation impact by wighting citations based on the total number of citations in a subject field.
See more