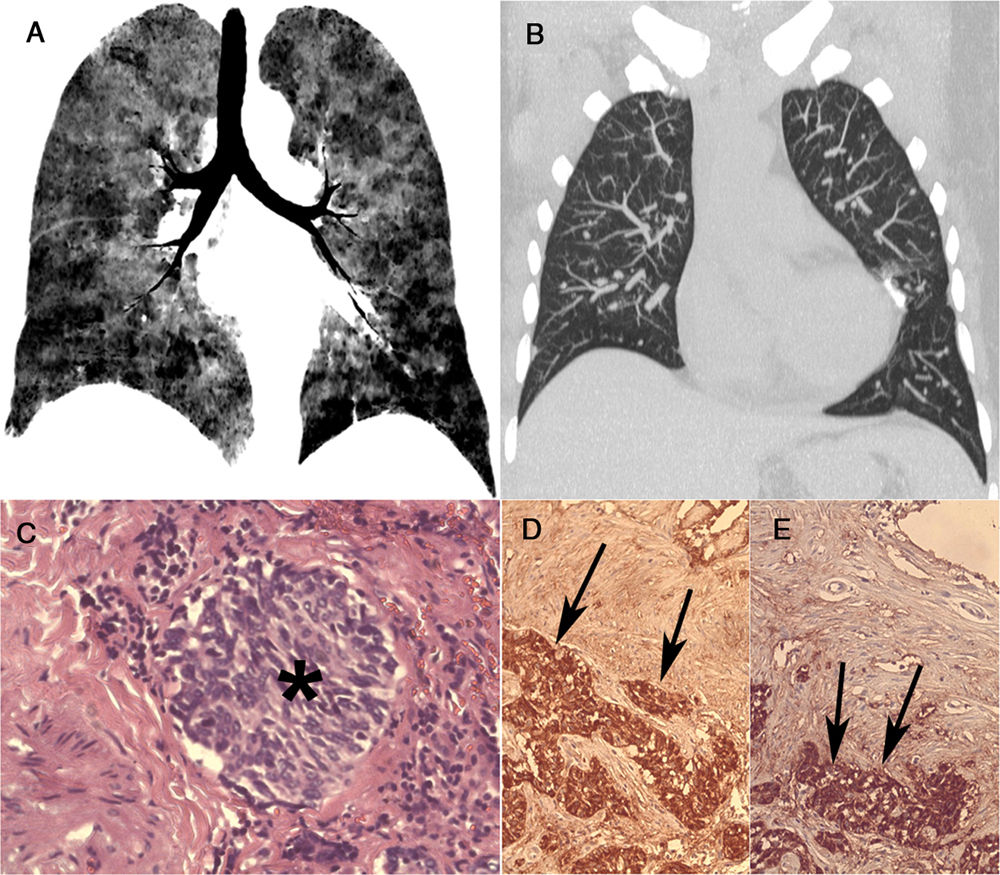
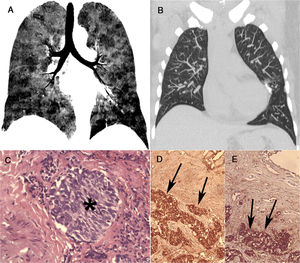
A 66-year-old nonsmoking woman presented with chronic dry cough, wheezing and dyspnea. She had previously been diagnosed with bronchial asthma. Chest computed tomography (CT) showed multiple bilateral small nodules and a diffuse mosaic attenuation pattern (Fig. 1A and B). Pulmonary function tests demonstrated an obstructive ventilatory pattern. Video-assisted thoracoscopic biopsy showed the proliferation of small, pale staining cells. Immunohistochemical staining revealed synaptophysin and chromogranin A positivity (Fig. 1C–E), supporting the diagnosis of diffuse idiopathic pulmonary neuroendocrine cell hyperplasia (DIPNECH).
A coronal minimum-intensity projection reformatted image (A) demonstrates mosaic attenuation with sharply defined lobular areas of low attenuation due to small airway obstruction (consistent with air trapping). A coronal maximum-intensity projection image (B) shows multiple bilateral small nodules, probably corresponding to tumorlets. A histopathological section (C) demonstrates a nodular aggregate (tumorlet) (asterisk) of atypical oval cells (hematoxylin and eosin staining, ×100). The tumoral cells expressed immunohistochemical positivity for synaptophysin (arrows) (D) and chromogranin A (arrows) (E), characterizing neuroendocrine cell proliferation.
DIPNECH is characterized by respiratory symptoms (cough, dyspnea and wheezing), airflow obstruction, mosaic attenuation with air trapping on chest CT, and often the nodular proliferation of neuroendocrine cells with or without tumorlets or carcinoid tumors on histology. Its diagnosis is more difficult in asymptomatic patients, especially those undergoing CT for cancer follow-up, in whom nodules must not be mistaken for diffuse lung metastases.1,2 In the appropriate clinical (e.g., middle-aged nonsmoking women with obstructive ventilatory defects) and radiological (e.g., combination of small nodules, features of constrictive bronchiolitis and mosaic attenuation) settings, the diagnosis of DIPNECH syndrome may be suggested. However, its confirmation requires histopathological analysis. On immunohistochemistry, the lesions express the most common markers of neuroendocrine cells, particularly chromogranin A and synaptophysin.1,2