Chylothorax (CTx) is an uncommon disease caused by extravasation of lymph fluid to the pleural cavity. Diagnosis is based on the detection of triglycerides or chylomicrons in pleural fluid. Triglyceride concentrations higher than 110mg/dl or the presence of chylomicrons are indicative of CTx.1 Etiology is defined as traumatic or non-traumatic, the most common causes of which are iatrogenesis or malignancy.2 Treatment can be conservative in the case of low-output CTx, or surgery may be necessary if disease is high-output or refractory.3 Prognosis depends on the underlying cause.
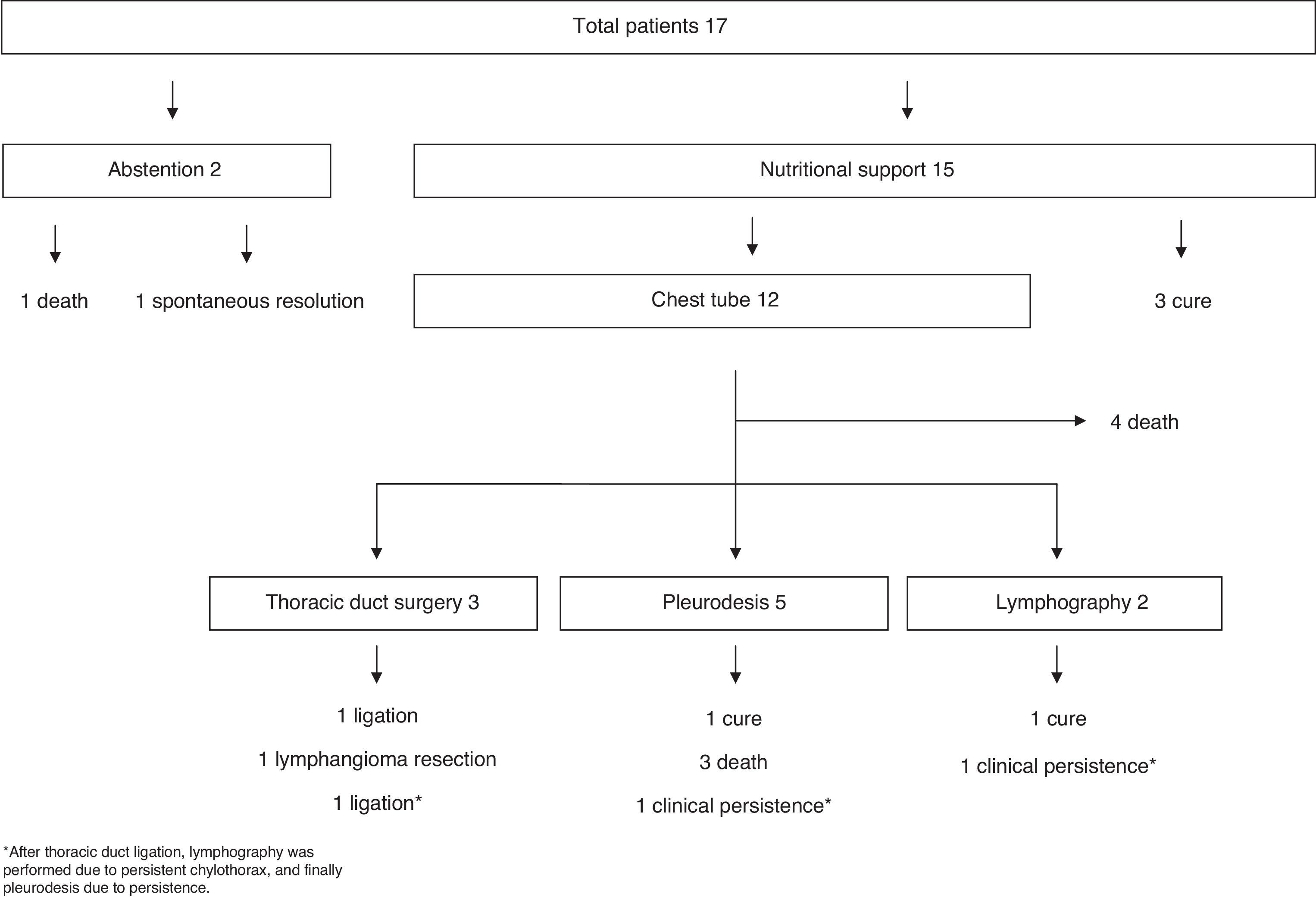
We reviewed 1600 cases of pleural effusion seen in our hospital between January 2010 and December 2013, and selected patients with triglyceride levels higher than 110mg/dl. We analyzed the etiology, clinical manifestations, diagnosis, and treatment of these cases, and reviewed the literature. Seventeen patients were found to have CTx (1.1%). Mean age was 64 (36–81) years, and 8 were men. The most common symptoms were dyspnea (7 cases), cough (3), ascites (3), and anorexia, asthenia and weight loss (4). Pleural effusion was right-sided in 8, left-sided in 2, and bilateral in 7. Pleural fluid obtained from 16 patients was milky in appearance and serous in 1; 12 were exudate, and 4 were transudate (data missing in 1 case). Etiology was non-traumatic in 13 cases, 11 of which were due to malignant disease, mainly lymphoma (n=5). One case was due to lymphangioma, and another was idiopathic. Of the remaining 4, 3 were caused by surgery and 1 by childbirth. With regard to treatment (Fig. 1), nutritional support was administered, with lipid restriction and medium-chain triglyceride diet in all patients, except 2 (due to death and spontaneous resolution). Pleural drainage was applied in 12 patients, and 5 underwent pleurodesis. Three required surgery (thoracic duct ligation), and 2 lymphography. Octreotide was administered in 3 cases, but results were unsatisfactory: 1 patient developed a skin rash, so it was discontinued, and other measures were required in the other 2 due to persistent effusion. Eight of the 17 cases died, 7 due to malignancy.
CTx is a rare entity, mainly caused by rupture of the thoracic duct and accumulation of chyle in the pleural cavity, or leakage from the peritoneum. Etiology of CTx is classified as traumatic or non-traumatic, the former being the most common, accounting for up to 50% of cases.4,5 In our study, the predominant etiology was non-traumatic. Traumatic etiologies can be subcategorized as iatrogenic (surgical acts such as esophagectomy) and non-iatrogenic (traumatism, childbirth labor, etc.).2 Neoplasic processes, predominantly lymphoma, are the most common non-traumatic cause. The most common symptoms are cough, dyspnea, and chest pain. Fever is less common, since chyle is a non-inflammatory fluid.5 Our series notably included 4 cases of anorexia, asthenia and weight loss, most likely due to the high rate of malignant diseases. Diagnosis is based on analysis of pleural fluid, which has been defined as milky or opalescent, but serous and bloody serous specimens have been described, and are even predominant in some series.1 In biochemical terms, this is a lymphocytic exudate with low LDH levels, although previous studies have described transudates in 32% of cases, mostly due to hepatic cirrhosis, nephrotic syndrome, and heart failure, among others.5 In our series, 4 were transudates due to malignancy. Most CTx are unilateral.4 In our series, 7 were bilateral and 10 were unilateral. CT must be performed if the cause is unknown. Other techniques for locating the lesion are lymphography and lymphoscintigraphy, but these techniques may cause adverse effects, and are of most benefit in patients in whom surgical repair is planned. Treatment of CTx will vary depending on severity and refractoriness. In low-output effusions, a lipid-free diet with medium-chain fatty acids is recommended. In more severe cases, fasting with total parenteral nutrition and pleural drainage is recommended. Since 1990, these conservative medical treatment modalities have been combined with somatostatin or its synthetic analog, octreotide, an effective strategy with a response rate of up to 80%, mainly in postsurgical CTx.6–8 These products are thought to act by reducing gastrointestinal blood flow, inhibiting gut motility and reducing lymphatic flow, leading to a reduction in the intestinal production of chyle.2 In our series, however, this treatment was ineffective or had to be discontinued due to adverse effects in the 3 patients who received it, although we must point out that none of these cases were postsurgical. Pleurodesis is a good option in persistent cases.2 Surgery is necessary in refractory or high-output CTx. Thoracic duct ligation has been shown to be effective 67%–100% of the time,3 but patients who are not candidates for this intervention may receive a pleuroperitoneal or pleurovenous shunt2,3 or thoracic duct embolization, although outcomes are variable.2 In our series, 15 patients received nutritional support, and 12 required an endothoracic tube. Three thoracic duct ligations and 2 lymphographies were performed, with CTx resolution in all cases.
In conclusion, CTx is a rare entity, diagnosed by the detection of chylomicrons or triglycerides >110mg/dl in the pleural fluid. Surgical interventions and lymphoproliferative diseases are the main causes. In low-output CTx, nutritional support and repeated thoracocentesis are generally effective, but cases of persistent or high-output CTx may require invasive techniques.
Please cite this article as: García J, Alemán C, Jáuregui A, Vázquez A, Persiva Ó, Fernández de Sevilla T. Quilotórax en adultos. Revisión de la literatura a partir de una serie de 17 casos. Arch Bronconeumol. 2017;53:407–408.