Three percent of rare diseases are pneumopathies. Improvements in survival and quality of life have led to a new situation where patients with rare respiratory diseases want to plan their reproductive lives. The intention of this review is to present the experience accumulated in the field of reproductive health of these women.
In several rare respiratory diseases, a genetic base has been identified. The combination of preimplantation genetic diagnosis, assisted reproduction and molecular biology techniques enable embryos to be studied genetically before being transplanted into the uterus. Therefore, the risk for transmitting a certain disease or chromosome alteration may be avoided in high-risk couples, and prenatal diagnoses may be done by chorionic villus sampling or amniocentesis.
As a general rule, contraceptive methods should be personalized by evaluating the general state of female patients as well as their possibilities for pregnancy, complications and the future possibility of lung transplantation.
In lymphangioleiomyomatosis and primary pulmonary hypertension, pregnancy is considered a contraindication. In the former, there is a very high risk for pneumothorax and loss of lung function. In the latter, mortality reaches 33%. In cystic fibrosis, it is estimated that each year 4% of patients become pregnant and there is no observed loss in lung function.
There are special circumstances in childbirth that should be considered as well as specific anesthesia risks.
The present review suggests that while taking decision about contraceptive methods, pregnancy as a contraindication or conditions for managing a pregnancy should be both individualized and multidisciplinary.
El 3% de las enfermedades raras son neumopatías. Las mejoras en la supervivencia y en la calidad de vida hacen que las pacientes con enfermedades respiratorias minoritarias deseen planificar su vida reproductiva. Esta revisión intenta presentar la experiencia acumulada en el campo de la salud reproductiva en estas mujeres.
En diversas enfermedades respiratorias minoritarias se ha identificado una base genética. La combinación del diagnóstico genético preimplantacional, la reproducción asistida y las técnicas de biología molecular permite realizar el estudio genético de los embriones, antes de ser transferidos al útero; por tanto, puede evitarse el riesgo de transmitir una determinada enfermedad o alteración cromosómica en las parejas de elevado riesgo y se puede, también, realizar un diagnóstico prenatal mediante biopsia corial o amniocentesis.
Como norma general, debemos personalizar el método anticonceptivo evaluando el estado general de la mujer y las posibilidades de embarazo, complicaciones y la posibilidad futura de trasplante pulmonar.
En la linfangioleiomiomatosis y la hipertensión pulmonar primaria el embarazo se considera contraindicado. En la primera existe un riesgo muy elevado de neumotórax y de pérdida de función pulmonar. En la segunda, la mortalidad alcanza el 33%. En fibrosis quística se estima que cada año un 4% de las pacientes se quedan embarazadas y no se observa un deterioro de la función pulmonar.
Existen circunstancias especiales en el parto a tener en cuenta y riesgos anestésicos específicos.
La presente revisión sugiere que tanto la decisión sobre la anticoncepción como la contraindicación de un embarazo o las condiciones de su seguimiento deben ser individualizadas y multidisciplinares.
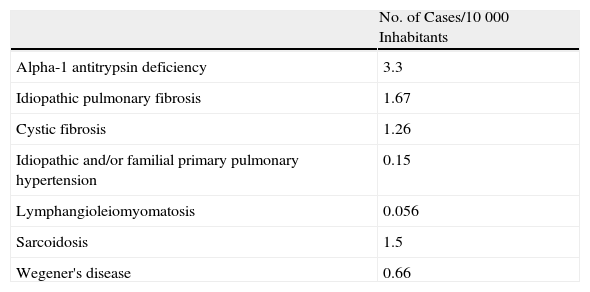
Rare or uncommon diseases are defined as those that have a prevalence of fewer than 5 cases per 10000 inhabitants. This definition was adopted by the “Programme of Community Action on Rare Diseases (1999–2003)” and has been accepted by most member-states of the European Union. It is also used by the European Medicines Agency for declaring orphan drugs. There are close to 6000 diseases that are classified as rare, and 181 (3%) of them are pneumopathies. Table 1 demonstrates the prevalence of several of them.
Prevalence of Main RLDS.
| No. of Cases/10000 Inhabitants | |
| Alpha-1 antitrypsin deficiency | 3.3 |
| Idiopathic pulmonary fibrosis | 1.67 |
| Cystic fibrosis | 1.26 |
| Idiopathic and/or familial primary pulmonary hypertension | 0.15 |
| Lymphangioleiomyomatosis | 0.056 |
| Sarcoidosis | 1.5 |
| Wegener's disease | 0.66 |
What rare lung diseases (RLD) frequently have in common is that they affect young patients, are chronic in character, entail severe prognoses and are complex to diagnose and treat.
Spectacular improvements have been made in survival and quality of life in some of these diseases, such as cystic fibrosis (CF) or primary pulmonary hypertension (PPH), and the accumulated experience in lung transplantation guarantees optimal survival when other therapeutic options have been exhausted. These factors mean that pulmonologists and other specialists now have to face questions and patient situations that we did not have to face several years ago. A prime example of this is reproductive life planning which, in addition to being a key intervention in improved patient health, is a human right, as has been established by Spanish legislation and several international documents.1
This review presents the multidisciplinary experience accumulated in the area of reproductive health of women with RLD, in a practical, integrated manner.
Reproductive Counseling for Patients Affected by Rare Lung DiseasesIn most rare lung diseases, a genetic origin has been identified.2 Genetic counseling is necessary for parents whose first child is affected by one of these diseases and who may plan another pregnancy. Counseling is also needed for couples with a member who is either affected by the disease or is a carrier of the mutation.
Currently, by means of the combination of advances made in the fields of pre-implantation genetic diagnosis (PGD), assisted reproduction, and molecular biology techniques such as fluorescence in situ hybridization and polymerase chain reaction, embryos can be studied genetically before being implanted in the uterus. Therefore, the risk for transmitting a certain disease or chromosomal alteration may be avoided in high-risk couples. In those cases requiring urgent genetic counseling (unplanned pregnancy), prenatal diagnosis may be performed by either chorionic biopsy or amniocentesis.
PGD consists of the biopsy of one or two cells of the embryo (blastomeres) on the third day of in vitro development. It is able to detect chromosomal anomalies, mutations or genetic variations associated with monogenic diseases. In each in vitro fertilization procedure, only those embryos that are determined to be healthy, chromosomally normal or, in recessive diseases, and non-diseased (although they may be carriers of the disease) are chosen to be transferred to the maternal uterus.
The first pregnancy of a CF-free fetus achieved by PGD in the world was published in 1992, and ten years later this was achieved in Spain.3 Although there are many CFTR mutations identified, and some have no clinical significance, it is advisable to carry out the gene study in patients with CF and in their families in order to identify the specific mutations in each case and to adjust the technique.
The European Society of Human Reproduction and Embryology (ESHRE consortium) has compiled a list of monogenic diseases that are analyzable with PGD. Briefly, they have identified mutations that provide genetic diagnoses for: alpha-1-antitrypsin deficiency (AAT) (E264V allele S, E343K allele Z in the PI gene); familial primary pulmonary hypertension (PPH), and lymphangioleiomyomatosis (LAM) associated with tuberous sclerosis. PPH (BMPR2 gene) is a dominant autosomal disease with reduced penetrance (20%), which means that, despite the fact that the risk of inheriting the mutation from an affected parent is 50%; the probability of developing the clinical disease may only be 10%. LAM associated with tuberous sclerosis presents a dominant autosomal inheritance in which mutations have been identified in two TSC1 and TSC2 genes for which there are DNA tests available for the PGD.
In the cases in which genetic tests are not predictive of disease but instead of risk, performing PGD requires the express authorization of health authorities and a report from the National Commission of Assisted Human Reproduction, which individually evaluates each case. The report of the Health Technologies Evaluation Agency of the Carlos III Health Institute and the Spanish Health Ministry (“Investigación priorizada en Evaluación de Tecnologías Sanitarias: [Inventario de Laboratorios de Análisis Genético Molecular en España]” Madrid: AETS – Instituto de Salud Carlos III, Madrid. Diciembre de 2004) has compiled a list of diseases and available centers in our country.4
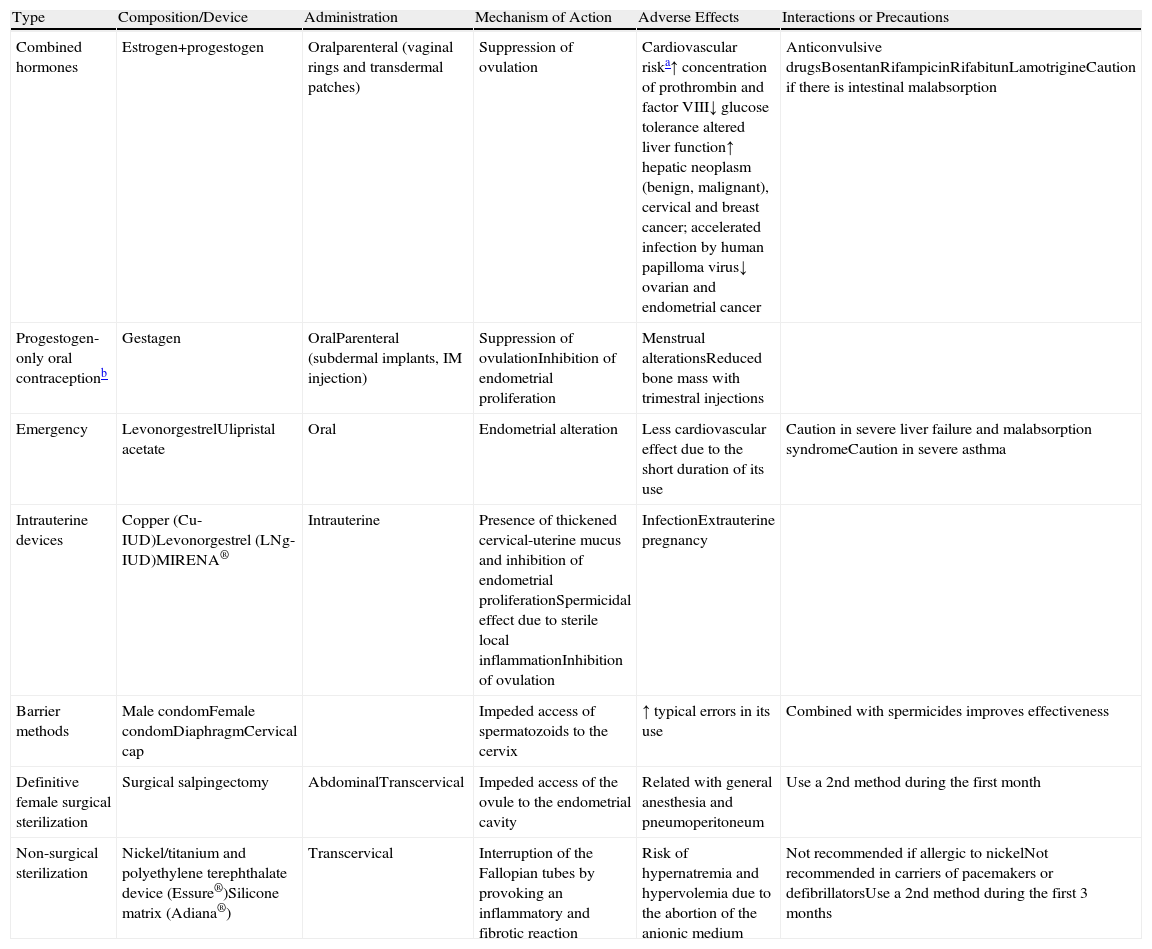
Family Planning in Women With Rare Lung DiseasesThere are few data reported about the best contraceptive methods for these lung diseases; not even the World Health Organization include these patient groups in their reviews. As a general rule, the method should be personalized and take into account the general state of each patient, her possibilities for pregnancy and possible complications.5Table 2 shows the contraceptive methods that are available and their main characteristics.
Contraceptive Methods Available and Main Characteristics.
| Type | Composition/Device | Administration | Mechanism of Action | Adverse Effects | Interactions or Precautions |
| Combined hormones | Estrogen+progestogen | Oralparenteral (vaginal rings and transdermal patches) | Suppression of ovulation | Cardiovascular riska↑ concentration of prothrombin and factor VIII↓ glucose tolerance altered liver function↑ hepatic neoplasm (benign, malignant), cervical and breast cancer; accelerated infection by human papilloma virus↓ ovarian and endometrial cancer | Anticonvulsive drugsBosentanRifampicinRifabitunLamotrigineCaution if there is intestinal malabsorption |
| Progestogen-only oral contraceptionb | Gestagen | OralParenteral (subdermal implants, IM injection) | Suppression of ovulationInhibition of endometrial proliferation | Menstrual alterationsReduced bone mass with trimestral injections | |
| Emergency | LevonorgestrelUlipristal acetate | Oral | Endometrial alteration | Less cardiovascular effect due to the short duration of its use | Caution in severe liver failure and malabsorption syndromeCaution in severe asthma |
| Intrauterine devices | Copper (Cu-IUD)Levonorgestrel (LNg-IUD)MIRENA® | Intrauterine | Presence of thickened cervical-uterine mucus and inhibition of endometrial proliferationSpermicidal effect due to sterile local inflammationInhibition of ovulation | InfectionExtrauterine pregnancy | |
| Barrier methods | Male condomFemale condomDiaphragmCervical cap | Impeded access of spermatozoids to the cervix | ↑ typical errors in its use | Combined with spermicides improves effectiveness | |
| Definitive female surgical sterilization | Surgical salpingectomy | AbdominalTranscervical | Impeded access of the ovule to the endometrial cavity | Related with general anesthesia and pneumoperitoneum | Use a 2nd method during the first month |
| Non-surgical sterilization | Nickel/titanium and polyethylene terephthalate device (Essure®)Silicone matrix (Adiana®) | Transcervical | Interruption of the Fallopian tubes by provoking an inflammatory and fibrotic reaction | Risk of hypernatremia and hypervolemia due to the abortion of the anionic medium | Not recommended if allergic to nickelNot recommended in carriers of pacemakers or defibrillatorsUse a 2nd method during the first 3 months |
Condoms (both male and female) may be used by all patients.
Oral contraceptives may not be indicated in patients with either frequent diarrhea or poor absorption that would impede the assimilation of the product, such as in CF patients. Combined contraceptives would be contraindicated in patients with liver cirrhosis, as can occur in DAAT. There is a greater proportion of cases with coagulation alterations in CF, as well as a greater risk for recurrent thrombosis in those patients who have a central catheter.6 Progestogen-only contraceptives have a smaller risk of complications and are an option to keep in mind in these pathologies. In principle, none of these hormonal treatments are altered by wide-spectrum antibiotics, but there may be alterations with some anti-tuberculosis medications. Trimestral injections of progestogen can reduce bone mass and are therefore not advisable in patients at risk for osteoporosis.
Intrauterine devices with levonorgestrel (LNg-IUD: Mirena®) and with copper (Cu-IUD) can be a good alternative for patients who desire safe, effective and reversible contraception. Failure rates are similar to definitive sterilization. LNg-IUDs release a small daily quantity of levonorgestrel and, although the effect is local and the quantity of progestogen is minimal, there are no studies that guarantee lack of systemic effects, and therefore they have the same contraindications as gestagen-only hormonal contraceptives. IUDs entail a risk for pelvic infección, particularly in connection with the insertion of the device and, further ahead, is an added risk for sexually transmitted disease. This could limit its use in immunosuppressed women.
There are also Essure® and Adiana® devices that would be indicated in those women who, due to their pathology or its severity, pregnancy is absolutely contraindicated. In patients who continually take corticosteroids or immunosuppressants, the Essure® method should be opted for because the Adiana® method is contraindicated, possibly due to the possibility of not having a good tubal inflammatory response and thus a possible failure.
In CF, the use of combined hormonal contraception is accepted as long as other risk factors are ruled out, such as a history of venous thromboembolism, active hepatic disease or pulmonary hypertension. Cu-IUDs and LNg-IUDs are also indicated, as are progestogen implants.6
Hormone products are absolutely contraindicated in LAM. Administering exogenous estrogen could make the lung disease progress. There are no studies of progestogen-only contraceptives, even though progesterone is one of the classic treatments for the disease. In general, these women should be recommended barrier methods or Cu-IUDs. As pregnancy is also generally contraindicated, definitive sterilization by hysteroscopy should be recommended, which entails less risk.7
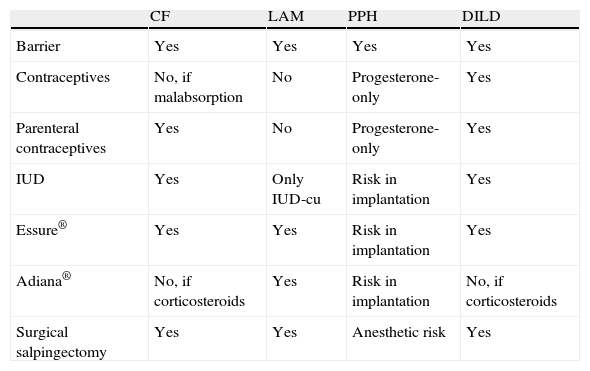
In pulmonary hypertension, pregnancy is contraindicated. Surgical sterilization is an option that has been successfully done, although with a mortality that can reach 6% in cases of open surgery. Laparoscopic ligature also presents anesthetic risk. Hysteroscopic sterilization seems to be the safest method in these cases. Other possibilities are LNg-IUDs (also Cu-IUDs) and subdermal progestogen implants. Nevertheless, the placement of an IUD or hysteroscopy may produce a vagal reaction that is not free from risk; therefore, these should only be done if there are no other possibilities while the patient is monitored. Combined hormone contraceptives are contraindicated, but progestogen-only contraceptives could be considered as they are also simultaneously permitted with anti-coagulant treatment. Thus, the best contraceptive methods are intrauterine devices (Mirena®) and contraceptive drugs that only contain progesterone.8Table 3 summarizes the indications of the different contraceptives in RLD.
Indications for Contraceptive Methods in ERM.
| CF | LAM | PPH | DILD | |
| Barrier | Yes | Yes | Yes | Yes |
| Contraceptives | No, if malabsorption | No | Progesterone-only | Yes |
| Parenteral contraceptives | Yes | No | Progesterone-only | Yes |
| IUD | Yes | Only IUD-cu | Risk in implantation | Yes |
| Essure® | Yes | Yes | Risk in implantation | Yes |
| Adiana® | No, if corticosteroids | Yes | Risk in implantation | No, if corticosteroids |
| Surgical salpingectomy | Yes | Yes | Anesthetic risk | Yes |
CF, cystic fibrosis; LAM, lymphangioleiomyomatosis; PPH, primary pulmonary hypertension; DILD, diffuse interstitial lung disease; C, contraceptives; IUD, intrauterine device.
It is important to take into account the future possibility of lung transplantation when choosing a contraceptive method. There are no specific references about contraception in women who undergo lung transplantation. It is logical to think that the risks for pulmonary thromboembolism should be avoided, and therefore combined hormone contraceptives should possibly be avoided. Barrier methods, definitive sterilization and possibly gestagen-only hormonal methods are options to be considered in these patients. Lastly, vasectomy is a definitive male sterilization technique that could be considered for spouses/partners of women with RLD. Nevertheless, many women with these pathologies have a life expectancy that is shorter than their sexual partners, and therefore this circumstance should also be evaluated.
Implications of Interstitial Diseases in Reproductive PlanningDiffuse interstitial lung disease (ILD) is a group of diseases that have a common denominator of interstitial lung affectation that differ in their physiopathologies and present, therefore, different clinical, evolutive and prognostic characteristics. Several entities may present problems associated with pregnancy and labor, among these sarcoidosis, cryptogenic organizing pneumonia, pulmonary fibrosis associated with connective tissue disease, Langerhans disease or vasculitis (Wegener, Goodpasture), mainly related with the maternal risks derived from hypoxemia due to higher oxygen consumption (fetal immaturity, pre-term labor) or systemic corticoid treatment in severe cases. Within this group, LAM merits special attention as it occurs mainly in women of child-bearing age. Symptoms can include dyspnea upon exertion, pneumothorax (frequently repetitive), chylothorax, hemoptysis or dry cough. Extrapulmonary involvement may include lymphadenopathies, chylous ascites, uterine fibroids and renal angiomyolipomas, although the clinical evolution is very variable.
Initially, theories were developed about the estrogenic influence in anomalous smooth muscle proliferation that characterizes lesions presented by patients, although radical anti-estrogen treatments have not been shown to be effective. As for pregnancy and childbirth, up to 67% develop pneumothorax and 47% present preterm labor, along with a decline in lung function parameters (FEV1, FVC and DLCO) in practically all cases in the post-partum follow-up, which makes pregnancy unadvisable even in mild cases.7,9,10
The emerging therapies proposed for LAM, like rapamycin or beta-blockers, should also be considered a problem for gestation, given the possible teratogenic effects that they entail.
Implications of Cystic Fibrosis in Reproductive PlanningCF is caused by mutations in a gene situated on the long arm of chromosome 7, and some 1800 possible mutations have been reported.11 This gene codifies the synthesis of the CFTR protein. Its absence produces an anomaly in ionic transport, which gives rise to the production of some particularly viscous secretions. The most relevant clinical manifestations are: bronchiectasis, sinusitis and nasosinusal polyposis; digestive malabsorption syndrome secondary to exocrine pancreatic insufficiency, meconium ileus, distal intestinal obstruction syndrome, hepatopathy and chronic pancreatitis; endocrine-metabolic alterations like diabetes mellitus and osteoporosis. Other manifestations include dehydration due to a loss of ions with sweat, or masculine infertility due to atresia or bilateral obstruction of the deferent ducts.
Current life expectancy is 35.9 years. Since 1991, the patient register of the “North American Cystic Fibrosis Foundation” estimates that 4% of women with CF over the age of 18 become pregnant annually.
Recommendations for preconception, gestation, labor and post-partum have been recently published by the European Cystic Fibrosis Society.12
The data analysis from the CF patient cohort suggests that pregnancy does not increase maternal mortality nor does it accelerate lung function deterioration, but during gestation both the use of antibiotics and hospitalizations increase. As for the fetus, there is a greater risk for prematurity, especially in women with low lung function levels and diabetes.13
Pregnancy is not recommended when there is a poor nutritional state in the mother, severe pulmonary disease, infection by Burkholderia cenocepacia and multivorans, cor pulmonale, severe hepatic disease or poorly controlled diabetes mellitus.
During pregnancy, the majority of the medication that is usually used in CF can be maintained: pancreatic ferments, liposoluble vitamins, bronchodilators, 7% saline solution, dornase alpha, azithromycin, vitamin A (limit of 10000IU/day due to risk for teratogenicity). Respiratory physiotherapy is recommended at least twice daily. Likewise, treatment compliance should be closely monitored.
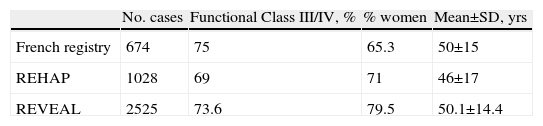
Implications of Pulmonary Hypertension in Reproductive PlanningPulmonary hypertension is a rare disease with high morbidity and mortality whose diagnosis is defined by the hemodynamic confirmation of a mean pulmonary arterial pressure (PAPm) higher than 25mmHg at rest, and more than 30mmHg while exercising. It predominantly affects women with a mean age of around 50 (Table 4) and a high percentage of women of childbearing age.14–16
General Demographic Data in Different Registries.
| No. cases | Functional Class III/IV, % | % women | Mean±SD, yrs | |
| French registry | 674 | 75 | 65.3 | 50±15 |
| REHAP | 1028 | 69 | 71 | 46±17 |
| REVEAL | 2525 | 73.6 | 79.5 | 50.1±14.4 |
REHAP, Spanish pulmonary arterial hypertension registry; REVEAL, registry to evaluate early and long-term pulmonary arterial hypertension disease management.
Physiological changes that occur in the circulatory system during pregnancy (increased plasma volume, cardiac output especially during labor and hypercoagulability), together with the presence of high pulmonary vascular resistances (PVR) typical of the disease, may alter the fragile hemodynamic balance of these patients and cause an acute increase in PAP and right ventricular failure.
PH of group II associated with mitral stenosis can entail special severity due to the risk of pulmonary congestion.
Mortality of pregnant patients with PPH reaches 33%, mainly during the first month post-partum. It is related with portopulmonary hypertension in particular and associated with connective tissue diseases and the use of general anesthesia. Therefore, in cases of pregnancy, abortion should be considered as early on as possible. Patients who respond to calcium antagonists with normalization of pulmonary pressure and are in functional class I are the only subgroup in which pregnancy has an acceptable risk.
Pregnancy patients should be referred to reference centers and have continuous access to expert professionals. Treatment of pregnant women with PPH should include: reduced physical activity; supplemental oxygen in case of respiratory failure and medication including beta-blockers to lower heart rate; diuretics to reduce the volume overload, initially at low doses; anticoagulation with low molecular weight heparin (the use of coumarin anticoagulants is not recommendable due to the risk for teratogenesis).
If PH is diagnosed during pregnancy, the specific treatment should be initiated early. This may include analogs of prostacyclin (iloprost and treprostinil), phosphodiesterase inhibitors (sildenafil, tadalafil), and calcium antagonists (nifedipine, diltiazem). Endothelin receptor antagonists are not recommended due to their potential teratogen power. Patients in functional class III/IV should receive continuous IV epoprostenol. If drug treatment does not control the symptoms or the patient was already in functional class III–IV before pregnancy, percutaneous valvuloplasty could be considered.17
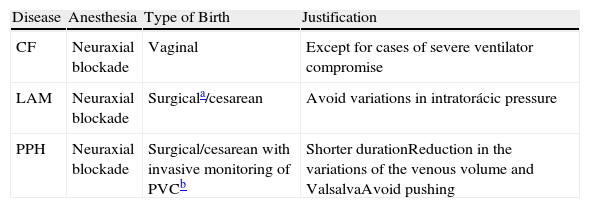
Morbidity and Mortality Associated With Childbirth in Pregnant Subjects With Rare Lung DiseasesIn the case of patients with RLD, childbirth is considered high risk and should be monitored by an experienced multidisciplinary team as it requires detailed planning and generally requires scheduled birth or cesarean section (Table 5).
The Authors’ Recommendations for Childbirth.
| Disease | Anesthesia | Type of Birth | Justification |
| CF | Neuraxial blockade | Vaginal | Except for cases of severe ventilator compromise |
| LAM | Neuraxial blockade | Surgicala/cesarean | Avoid variations in intratorácic pressure |
| PPH | Neuraxial blockade | Surgical/cesarean with invasive monitoring of PVCb | Shorter durationReduction in the variations of the venous volume and ValsalvaAvoid pushing |
The objective of induction is to achieve a state of uterine dynamics that is effective for vaginal birth. To do so, cervical maturation can be favored with E2 prostaglandins and induction with oxytocin. Oxytocin has an anti-diuretic effect, increases pulmonary vascular resistance, and reduces systemic vascular resistance. Therefore, it is essential to adequately manage the hydroelectrolytic balance and to use lowest possible dosage.
Scheduled C-sectionThis is indicated when the obstetrical conditions are not favorable or when the maternal or fetal state does not make a vaginal birth possible. C-sections before week 34 of gestation require acceleration of fetal lung maturation with betamethasone administered to the mother. A Misgav-Ladach-type surgical dissection technique is recommended to reduce bleeding, and the use of long-acting oxytocin analogs (duratobal) is recommended to prevent uterine atony.
Special SituationsThreat of Pre-term LaborThis is a frequent complication in pregnant women with an RLD. Their treatment consists of the administration of tocolytics: atosiban with less risk for acute pulmonary edema (PE) or oral nifedipine, with no risk for acute PE.
Pulmonary HypertensionUterine contractions may increase cardiac output (CO) up to 25%. In addition to CO, the stress and exertion during the expulsion period of labor increase sympathetic tone and with it the myocardial consumption of oxygen that may precipitate the failure and claudication of the right ventricle. Therefore, it is important to maintain proper pre-load levels of the right ventricle and after-load of the left ventricle.
Immediate post partum is the most critical phase due to the fact that there is an abrupt increase in pulmonary vascular resistance. Most deaths occur around the 7–9th days after childbirth. Therefore, these patients should remain in the intensive care unit in order to control the decline in PVR with fast-acting vasodilators (nitric oxide, inhaled iloprost or epoprostenol) supported with inotropes (dobutamine or noradrenaline) to avoid the dysfunction of the right ventricle related with the increase in volume or the existence of anemia.
In clinical practice, scheduled cesarean sections with local anesthesia are usually done in weeks 32–34 to avoid emergency situations.18
PneumothoraxThis complication may occur in pregnant women with LAM or CF. If pneumothorax occurs during labor, a pleural drain should be inserted until definitive surgical treatment can be carried out. In women with bilateral pleurodesis or pleurectomy, a surgical birth is not necessary.
Anesthesia in Patients With Primary Pulmonary HypertensionThe anesthetic procedure is especially complex in pregnant women with PPH. Described below are some recommendations in this regard (Table 6):
- -
Systemic arterial hypotension should always be avoided as it compromises coronary perfusion and right ventricular function.
- -
Always maintain adequate preload.
- -
Precisely monitor heart rate because an elevated rate may precipitate acute right heart failure and increased myocardial oxygen consumption.
- -
Maintain optimal hematocrit, fraction of inspired oxygen (FiO2), and hemoglobin levels to enable adequate oxygen extraction.
- -
Avoid hypoxemia, hypercapnia and acidosis, as they are the most powerful stimuli for increasing pulmonary vascular resistance.
- -
Maintain careful control of anti-coagulation with low molecular weight heparin to minimize the risk of bleeding and epidural hematoma.
- -
It is fundamental to monitor the following: invasive monitoring with a catheter in the pulmonary artery of arterial pressure, high-flow venous pathway, transesophageal ultrasound, and central temperature.
- -
Administer selective pulmonary vasodilators to maintain CO.19 An inotropic (milrinone or dobutamine) should be initiated and, when an acceptable CO is reached, a selective lung vasodilator may be started (inhaled nitrous oxide). Prostacyclin (PGI2) is a powerful vasodilator with antiplatelet effects. The oral form is contraindicated during gestation. The intravenous form, epoprostenol, is considered the drug of choice when it is necessary to reduce right ventricular afterload, although the side effects limit its administration.20 Its synthetic analogue, iloprost 16, is simpler to administer and does not affect RVS. Calcium antagonists are used only when there is a demonstrated reduction in pulmonary vascular resistance with proper CO. There is little experience during pregnancy with type V phosphodiesterase inhibitors (e.g. Sildenafil). In the case of systemic arterial hypotension, the agent of choice is noradrenaline. Levosimendan is starting to be used for cardiac preconditioning in patients with low ejection fraction who are scheduled for non-cardiac surgery. There are few publications of its use in pregnant women, but in vitro it has been seen to reduce uterine dynamics. Finally, non-depolarizing relaxants should be preferred, as they have less potential for releasing histamine, which induces systemic arterial hypotension. Vasopressin, a systemic adrenergic vasoconstrictor with possible pulmonary vasodilator properties, may have advantages over other vasopressors for treating hypotension after childbirth. It is a powerful uterine vasoconstrictor and is therefore not used before labor, but increased uterine tone after childbirth is beneficial. Post-op pain control is also an important aspect in patient care in order to avoid increased pulmonary arterial pressure.
Considerations About Anesthesia in PPH.
| • Minimize the hemodynamic effects secondary to laryngoscope with opioids |
| • Titer inhalation agents in detail due to their negative inotropic effect |
| • Avoid the use of nitrous oxide |
| • Avoid the use of PEEP and high airway pressure |
PPH, primary pulmonary hypertension; PEEP, positive end-expiratory pressure.
There is limited experience in the reproductive health of women with RLD. This circumstance complicates patient management while at the same time being an important challenge. One of the fundamental objectives of medical care in severe chronic diseases is improved quality of life, and this concept obviously includes patients’ sexual and reproductive lives.
In rare diseases, by definition the number of affected individuals is not large. Therefore, clinical assays that would be able to certify the scientific evidence from interventions are very difficult and/or have impossible frequencies. Circumstances such as pregnancy in women with RLD or transplantation are currently anecdotal cases or small series, so making recommendations is very difficult.
The present review suggests that both the decision about the best contraception as well as the contraindication of pregnancy or the conditions of its follow-up and outcome should be individualized and assessed in a multidisciplinary manner. Although there are guidelines for some specific cases, in general the recommendations of experts are the highest degree of evidence found.
Clinical registries have been demonstrated to be of great use in order to increase our knowledge about the natural history and interventions in rare diseases. The incorporation in these registries of data compiled about contraceptives and pregnancies in RLD could provide specific information for the follow-up of patients who in the near future will want to be able to enjoy near-normal reproductive health.
Conflict of InterestThe authors declare no conflicts of interest.